While the College motto is generally regarded as applying to the process of normal birth, it is also an appropriate reference to the history of colposcopy. Much of the research that underpins our current understanding of cervical pathology took place in the concentration camps of Nazi Germany.
The history of colposcopy begins in Hamburg, Germany, in the early 1920s. German gynaecologists were beginning to understand that cancer of the cervix might have a precursor condition, which they termed ‘carcinomatous surface coating’. In 1921, the professor of gynaecology at Hamburg University, Von Franqué, assigned his assistant, Hans Hinselmann, to the study of this cervical surface. In particular, he advised him to look at the leukoplakias that, it had already been observed, could be seen with the naked eye, adjacent to many small cervical cancers.
Hinselmann realised that to see these small lesions properly some magnification was needed. As he would later write: ‘the examination of the cervix and vagina with the unaided eye does not meet the demands of scientific appraisal. The use of magnification [is required].’ With the help of technicians from the Leitz Company, the predecessor of Leica, manufacturers of cameras and microscopes, he devised the first binocular colposcope. This was a cumbersome creation, but it enabled him to gain an excellent view of the cervical epithelium. However, instead of the tiny ulcer, surrounded by leukoplakia, that he had expected to find preceding cervical cancer, he discovered a range of distinctive surface appearances that reflected histological changes in the epithelial tissues beneath them. Thus began his lifelong study of the cervix and the development of the science and terminology used by colposcopists today.
Hinselmann published his first paper on colposcopy in 1925, and the first textbook of colposcopy in 1933; the latter included a description of mosaic patterns in lesions that Hinselmann recognised as pre-cancerous. In 1930, he became director of his own gynaecological clinic, the Frauenklinik Altona in Hamburg. Gynaecologist Dr Helmut Wirths, whose brother Eduard was also a doctor, worked with him.
In the years before the Second World War, gynaecologists in a number of countries became interested in colposcopy and in Hinselmann’s work. They included Babes in Romania; Levy, Emmert, Broders and Sacks in the USA; Usandizaga in Spain and Shaw in the UK. In the USA, Papanicolau’s work on vaginal cytology and its ability to detect cervical abnormalities was also gaining currency, although at first it seemed to clinicians that the two techniques were in competition rather than potentially complementary. Colposcopy was introduced to Argentina by Jakob in 1932. He established the first colposcopy clinic in South America, a part of the world where the techniques and science of colposcopy have flourished ever since.
By the late 1930s, a substantial number of US gynaecologists were taking an interest in the possibilities the colposcope offered. There were some reservations; in 1934 Sacks commented on ‘the cumbersome binocular endoscope of Hinselmann’. Another American, Gelhorn, in 1936 praised Hinselmann as having ‘added a new chapter to gynaecologic diagnosis’, but he also felt that: ‘the size, clumsiness and great expense of Hinselmann’s colposcope mitigates against its universal adoption.’ However Farrar, writing in 1938, pointed out that: ‘It takes time and patience to acquire skill with a new technique, and one must learn what a normal cervix looks like when viewed with low and then high magnification.’ Farrar was also one of the first writers in English to describe the transformation zone as the site of pre-malignant change: ‘Early carcinoma of the cervix…begins in the majority of cases in the unbroken epithelium of the external os on the borderline between the columnar epithelium of the cervical canal and the squamous epithelium of the portio, and spreads laterally. It is simple, white in color, and its borders are sharply defined from the adjacent tissue.’
Meanwhile, in Switzerland, Schiller in 1936 introduced the use of iodine, still often applied today to demarcate abnormal areas. Two years later Hinselmann himself described the use of acetic acid for the delineation of cervical abnormalities visible colposcopically. What prompted Hinselmann’s use of vinegar in this unorthodox way? My own theory is based on the fact that douching was at the time a common habit, particularly among European women, for reasons of ‘feminine hygiene’ and attempts at postcoital contraception. Dilute household vinegar was a product commonly used for this purpose. Very possibly Hinselmann observed in one or more patients who had followed this practice the characteristic changes in the epithelial appearances. The use of acetic acid rapidly spread and, in 1939, Kraatz, working in Germany, devised the green filter, through which abnormal areas painted with dilute acetate are even more clearly demarcated. In England, Shaw acquired a colposcope and began the practice of colposcopy in the UK.
During the Second World War, Hinselmann remained in his clinic in Hamburg, as did Helmut Wirths. Contact with colleagues in Allied countries ceased. Eduard Wirths had joined the Nazi party while still a medical student and, in 1934, he joined the SS. When the war began he was first sent to the Russian front, but after a heart attack was transferred as medical director first to Dachau concentration camp and then to Auschwitz. There is good evidence to show that under Eduard Wirths’ direction, a German-Jewish gynaecologist and prisoner, Maximilian Samuels, was compelled to perform colposcopies, using a Hinselmann colposcope, on Jewish women prisoners, take photos of the results, then remove the cervixes and despatch them to Hinselmann’s clinic in Hamburg. It would seem that Helmut Wirths was also involved in this process and that he visited his brother in Auschwitz and performed some colposcopies there.
After the war, Hinselmann was found guilty by the Allies of having conducted forced sterilisations on Gipsy women at the Altona clinic and sentenced to three years’ imprisonment. Viennese historian Ruth Jolanda Weinberger, who has conducted research into medical experimentation in Auschwitz using original documents from the camp hospital, has produced convincing evidence also linking Hinselmann to the study of the cervical tissues obtained from Auschwitz.

Figure 1. Colposcope 1970s from the RANZCOG Museum collection. Dr Mitchell used one half of a pair of field glasses and some ingenious welding techniques to create his unique instrument. Donation of Mrs Paul Mitchell, 1998.
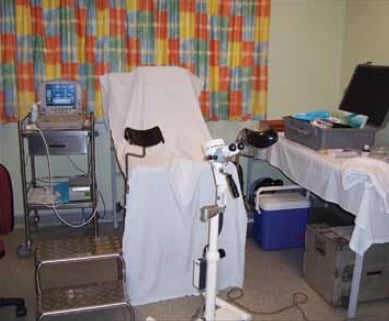
Figure 2. The FROGs travelling colposcope, which travels an average 1000km each working week.
With the war over, there was renewed interest in colposcopy in Europe and North America, and renewed contact with colposcopists in South America. Hinselmann himself seems to have been rehabilitated by the late 1940s; he made several visits to South America and one to Spain to lecture and teach the techniques. Bolten, who has been called ‘the father of modern colposcopy in the United States’, came to the USA in 1953 from Germany, where he had been trained in colposcopy. First in Philadelphia and then in New Orleans, he trained others who formed a nucleus that led to the foundation of the American Society for Colposcopy and Colpomicroscopy in 1964. By 1977, it was estimated that some 3000 US gynaecologists had been trained in colposcopy, and colposcopy became integrated into teaching programs for residents in gynaecology. By the mid 1950s it was becoming acknowledged both in the Americas and in Europe that cytology and colposcopy could be complementary techniques in the diagnosis of cervical pre-malignancy.
In 1956, Stallworthy at the Radcliffe in Oxford acquired a colposcope. Not long after, the young Malcolm Coppleson arrived from Sydney as a registrar, rapidly mastered the use of the instrument and began a career that included world eminence in the field of cervical pathology and its management. Coppleson’s first papers on the value of colposcopy in detecting precancerous lesions appeared in 1960; in 1967, he and Reid published a book on premalignant conditions of the cervix. In 1971, the first British colposcopy group was founded; in the same year Coppleson, Reid and Pixley published the first edition of their colposcopy text, which refined terminology and established the importance of the transformation zone. It was from this group that Australian colposcopy rapidly developed.
Not everyone could afford an elegant imported German colposcope for their private practice. Undaunted, Dr Paul Mitchell of Brisbane made his own (see Figure 1) – now part of the RANZCOG College Collection. Perhaps other examples of such gynaecological ingenuity lurk unacknowledged in garages across Australia.
Colposcopy now plays an integral role in Australian and New Zealand gynaecological practice, and is part of the training of all gynaecologists. The travelling colposcope (see Figure 2) of the Far North Queensland Obstetric and Gynaecological Service (FROGS) is just one example of the use of smaller, easily-portable instruments in practice in rural and remote parts of the country.
We are much indebted to the original work of Hinselmann. However, we should also pay attention to the words of Weinberger, who wrote in 2007:
‘Sixty-two years after the liberation of Auschwitz, the father of the colposcope remains a key figure in medical history, and for the untold number of lives he has saved he deserves credit. But for his complicity in the unbearable suffering inflicted on Jewish women in Auschwitz… Hinselmann deserves a qualified entry in the history books – and a moment of reflection from the millions of women who each year undergo a colposcopy.’
Further reading
Maclean JS. The life of Hans Hinselmann. Obstetrical and Gynecological
Survey 1979; 34 (11): 788-89.
Weese WH. A Brief History of Colposcopy. Journal of Reproductive Medicine 1976; 16 (5): 209-11.
Di Paola GR. History of the International Federation of Cervical Pathology and Colposcopy (IFCPC). European Journal of Gynaecological Oncology 2009; 30 (2): 117-123.
Torres JE, Riopelle MA. History of Colposcopy in the United States. Obstetrics and Gynecology Clinics of North America. 1993; 20 (1): 1–6.
Farrar LKP. The use of the colposcope and the Schiller test in the diagnosis of early or latent carcinoma of the cervix uteri. Surgical Clinics of North America. 1938; 18:523 9.
Weinberger RJ. The Deadly Origins of a Life-Saving Procedure. Forward, 26 January 2007. At http://www.forward.com/articles/9946 .
Weinberger RJ. Fertility experiments in Auschwitz-Birkenau – the perpetrators and their victims. Sudwestdeutscher Verlag fur Hochschulschriften AG, 2009.






Leave a Reply