An overview of current and future contraception options.
The range of contraceptive methods has expanded in the last few decades so that women, and their partners, are increasingly likely to find a method that is a ‘good fit’. However, the concept of what makes an ‘ideal contraceptive’ is by no means universal. While it may seem obvious that a contraceptive method should be effective, affordable and with minimal risks and side effects, other attributes such as reversibility, the possibility of detection by others and additional ‘non-contraceptive’ benefits may be desirable for some, but not for others. This article provides an overview of recent developments in contraception as well as a glimpse of what to expect in the future.
Australian women have been taking the combined oral contraceptive pill (COCP) since 1961, although somewhat astoundingly it was then only available to women who could prove that they were married! Early COCPs contained much higher hormone doses and had higher risks and more side effects. The quest has, therefore, been to reduce the hormonal dose while maintaining efficacy. While early pills had the equivalent of 150mcg of ethinyl estradiol (EE), today’s low-dose pills contain between 35 and 20mcg EE.
The most serious COCP-related risk is venous thromboembolism (VTE), a ‘hot topic’ in recent years. Estimates of the background rate of VTE in women of reproductive age who are neither pregnant nor postpartum vary from 0.7 to 13.5 per 10 000 women years1 and use of the COCP appears to increase the risk approximately two- to three-fold over baseline.2 When discussing VTE risk it is crucial to set the risk in context and explain that the absolute risk is extremely low, far lower for example than the VTE risk in the postpartum period.
While lowering the EE dose from 100 to 35mcg was definitively associated with a reduction in VTE risk, the effect of reducing EE yet further to 20mcg is less clear. Any potential safety benefits in relation to a reduction in EE dose also need to be weighed against the loss of cycle control that occurs as the oestrogen dose drops. Unpredictable bleeding is certainly a side effect that most women would rather avoid.
The effect of different progestogens on VTE risk is also unclear. COCPs containing the earliest progestogen, levonorgestrel (LNG), remain the ‘gold standard’ in relation to risk. Newer pills containing drospirenone have been under scrutiny recently. While studies are conflicting, on balance there appears to be an increased VTE risk with dropsirenone COCPs.3 However, the fact remains that the absolute risk for all the COCPs on the market is extremely low for women who are not contraindicated for the use of oestrogen. Until 2010 all COCPs contained EE, but this has now changed with the introduction of pills with oestradiol or its pro-drug, oestradiol valerate (marketed as Qlaira® and Zoely®, respectively). So what, if any, are the potential advantages of these newer pills? In the research setting, oestradiol-containing COCPs have a reduced impact on liver metabolism, including clotting factors.4,5 However, it is important to be aware that ‘real life’ evidence for any safety benefit over EE-containing pills is pending. Large post-marketing surveillance studies will provide observational data in a few years.
Some women may choose a particular COCP for its additional non-contraceptive benefits, for example, for acne control or reduction in heavy menstrual bleeding (HMB). However, evidence for the benefits of one pill type over another is generally lacking and finding the most appropriate COCP to suit an individual woman’s circumstances is often a matter of ‘trial and error’.
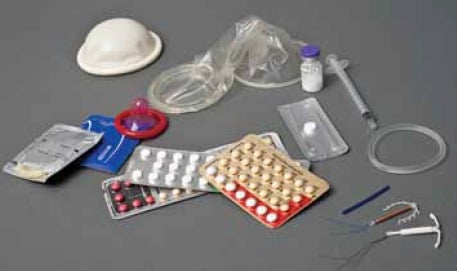
A selection of contraceptives – there is no one method that is suitable for all.
DMPA is given every three months, but can affect bone density.
While all COCPs will potentially reduce blood loss, as a result of a placebo-controlled trial showing a significant reduction in the duration and quantity of bleeding over 13 cycles, the oestradiol valerate/dienogest pill has gained an indication for the management of idiopathic HMB in women requiring contraception.6 This results from the potent endometrial effect of dienogest in combination with oestradiol valerate in a quadriphasic regimen with a shortened placebo break. This COCP may, therefore, be a suitable choice for appropriately investigated perimenopausal women (at least those who can afford its non-PBS listed cost). The dosing regimen also results in more complex ‘missed pill rules’ so it would not be an ideal choice for young women starting the pill for the first time.
Extended COCP regimens
When the COCP was first developed, the social context of the day demanded that it should ‘mimic the natural cycle’ with a guaranteed monthly withdrawal bleed. Women have been pretty much stuck with this outdated concept ever since, with most pill packs providing 21 hormonal and seven placebo pills. This is now changing with the advent of COCPs with either four placebos (Yaz® and Zoely) or two placebos (Qlaira). Why is reducing the placebo break useful? Apart from potentially reducing the duration and quantity of withdrawal bleeding, it can also reduce hormonal withdrawal symptoms such as pelvic pain and headache and provide a greater ‘margin for error’ if pills are forgotten at the beginning of the next pack.
Many women have been skipping their placebo pills for years in order to avoid withdrawal bleeds and the practice of running three pill packs together without placebos is well documented. Extended cycle packs with either 84 hormone and seven placebo pills or 365 hormone and no placebo pills are available in other countries and prolonged use of the pill for up to 12 months has been shown to be both safe and acceptable.7 Family Planning NSW is also comparing continuous use of low-dose pills or vaginal rings (replaced every four weeks) in a ‘bleeding-signalled regimen’ until four days of continuous spotting and/or bleeding occurs at which time the pill is stopped or ring removed on the fifth day and restarted five days later. Trial results, including bleeding patterns and acceptability, will be available in 2013.
Vaginal rings and patches
The vaginal ring offers an alternative contraceptive delivery system that is acceptable to women, although use may be limited by cost as it is not available on the PBS. The vaginal ring (available as NuvaRing®) allows for a reduction in EE dose to the equivalent of 15mcg per day, although this does not translate into a reduced VTE risk. Women can hook up to an SMS reminder system for removal and reinsertion timing – contraceptive apps are definitely the way of the future!
‘Back to back’ removal and immediate reinsertion of the ring every three to four weeks is useful for women choosing to avoid withdrawal bleeding. A Population Council multinational trial of a vaginal ring containing sufficient hormones for 12 months of use will hopefully result in the availability of this useful product in the not-too-distant future.
Contraceptive patches are unavailable in Australia, except in our research setting. Again, despite their low-dose of hormones, they are not associated with a reduced risk of VTE.
The era of LARCs
Long-acting reversible contraceptives (LARCs) are methods administered less frequently than once a month. Since they are independent of the need to remember to ‘do something’ at the time of intercourse or on a daily basis, their ‘typical use’ effectiveness is close or identical to their effectiveness under research conditions.
The earliest LARCs are the injectables, principally depot medroxyprogesterone acetate (DMPA) given every three months. DMPA remains a useful method of contraception as it is effective, cheap and undetectable by others. That said, DMPA has had its detractors over the years in relation to its bone density effects (reversible in women of mid-reproductive age and not related to an increase in fracture risk) and the fact it is not immediately reversible. New approaches including reduced hormonal doses as well as subcutaneous delivery methods may be the way of the future.
Contraceptive implants
Contraceptive implants provide highly effective, cost-effective and immediately reversible contraception for up to three years (with no significant impact on bone density). While implants have been available in Australia since 2001, 2011 saw the change from Implanon® to Implanon NXT®. The difference lies in the applicator, designed to minimise deep insertions leading to difficult and potentially risky removals. Implanon NXT also contains barium sulphate to allow for visualisation in the case of deep insertion (somewhat counterintuitive if the new applicator really does minimise deep insertions, but the intention is good).
Unacceptable vaginal bleeding is the most significant side effect and can lead to early removal. Frequent and/or prolonged heavy bleeding affects approximately one in five women.8 Women can be informed that the bleeding pattern in the first three months of use is broadly predictive for future bleeding patterns and that those with an unfavourable initial pattern have a 50 per cent chance of improvement.8 The evidence-base for the management of unacceptable bleeding patterns is limited and recommendations also follow a pragmatic approach.9,10 If not contraindicated, use of a COCP for up to six months (or longer if required) can provide a ‘band-aid’ solution for current bleeding, but will not have any long-term effect when stopped. Similarly, a five-day course of mefenamic acid or tranexamic acid may shorten the duration of a current bleeding episode, but will not affect the subsequent bleeding pattern.
Intrauterine devices
Intrauterine contraception has been available for decades, although the latest devices are a far cry from earlier prototypes such as the Dalkon Shield. It is certainly time to lay some of the misconceptions about intrauterine devices (IUDs) to rest. For example, the increased risk of pelvic infection is low and appears to be mainly confined to the first 20 days after insertion11,12 after which the risk reverts to the woman’s background risk for infection. There is no evidence of an increased risk of subsequent infertility for women using an IUD.13
Medicare data show that use of the LNG-releasing IUD (Mirena®) is increasing, presumably due to its delivery of highly effective, cost-effective contraception as well as its menstrual blood loss benefits. A smaller device that releases the equivalent of 12mcg rather than 20mcg of LNG per day is currently under trial. This new device, hopefully available in 2014, may prove especially suitable for young nulliparous women for whom the IUD is an acceptable and appropriate method of contraception.
Copper-IUDs, while less prevalent than the LNG-IUD, have a valuable place in the contraceptive arsenal for women requiring a highly effective long-acting hormone-free method. Copper-IUDs can also be used to provide postcoital emergency contraception for up to five days after unprotected intercourse. The practicalities of timely access in the primary care setting need to be addressed before their use in this context becomes a realistic proposition. However, family planning organisations are currently expanding their delivery of IUD-insertion training for GPs so hopefully these barriers will be reduced in the future.
Condoms and the importance of dual protection
Condoms, both male and female, are the only contraceptives that simultaneously protect against sexually transmissible infections (STIs). As a contraceptive method they have a failure rate of up to 18 per cent, mainly because of incorrect or non-use. For women at risk of STIs they can be ‘doubled up’ with another effective contraceptive method such as an IUD or implant. The only female condom available in Australia is made of polyurethane, but its use is limited by lack of availability and cost (approximately $3 each). Newer prototypes include a condom made of a nitrile polymer that optimistically promises ‘quieter use’.
Emergency contraception – new horizons
The most commonly used emergency contraceptive method is a single 1.5mg dose of LNG taken as soon as possible after unprotected intercourse. While almost all Australian women in a recent survey had heard of the emergency contraceptive pill (LNG-ECP), unfortunately fewer than half were aware that it was available without a prescription at the pharmacy.14
The LNG-ECP primarily acts to prevent or delay ovulation by interfering with follicular development and preventing the LH surge.15 It appears to have no effect once the LH surge has commenced. It is licensed for use up to 72 hours after unprotected intercourse, but WHO recommends it can be used up to five days after intercourse.16 While recent data suggest delaying administration until the fifth day increases the risk of pregnancy more than fivefold compared with administration within 24 hours17, the threshold for use should be low.
An alternative oral emergency contraceptive has been available in Europe since 2009, in the form of the selective progesterone receptor modulator, ulipristal acetate (UPA). UPA is marketed as ellaOne® and is licensed for use up to 120 hours after unprotected intercourse or contraceptive failure. It works primarily in the same way as the LNG-ECP by inhibiting or delaying ovulation, but also may cause alteration to the endometrium. Research suggests it has superior efficacy to the LNG-ECP at 24, 72 and 120 hours.18 Hopefully Australian women will be able to access UPA soon.
In conclusion
Since women may use contraception for approximately half of their lifetime, it is essential that we provide careful evidence-based advice about the variety of available options. The ‘best fit’ for an adolescent is likely to differ from the method chosen as a postnatal 32 year old and then, later, as a perimenopausal 49 year old.
New developments in technology coupled with well-designed research trials will help ensure that Australian women and their partners are able to find a contraceptive method that best suits their stage and situation in life.
Declaration of interest
Deborah Bateson has provided expert opinion for MSD and Bayer Healthcare as part of her role as medical director of Family Planning NSW. She has been supported to attend conferences by BayerHealthcare.
References
- Heinemann LA, Dinger JC. Range of published estimates of venous thromboembolism incidence in young women. Contraception.2007;75(5):328-36.
- Lidegaard O, Nielsen LH, Skovlund CW, et al. Risk of venous thromboembolism from use of oral contraceptives containing different progestogens and oestrogen doses: Danish cohort study, 2001-9. BMJ.2011;343:d6423.
- Parkin L, Sharples K, Hernandez RK, Jick SS. Risk of venous thromboembolism in users of oral contraceptives containing drospirenone or levonorgestrel: nested case-control study based on UK general Practice Research Database. BMJ. 2011;342:d2139.
- Parke S, Junge W, Mellinger I. Comparative effects of a four-phase regimen of estradiol Valerate/dienogest versus ethinylestradiol/levonorgestrel on haemostatic parameters. 24th Annual Meeting of theESHRE. 2008.
- Gaussem P, Alhenc-Gelas M, Thomas JL, et al. Haemostatic effects of a new combined oral contraceptive, nomegestrol acetate/17beta estradiol, compared with those of levonorgestrel/ethinyl estradiol. A double-blind, randomised study. Thromb Haemost. 2011;105(3):560-7.
- Jensen JT, Parke S, Mellinger U, et al. Effective treatment of heavy menstrual bleeding with estradiol valerate and dienogest: a randomized controlled trial. Obstet Gynecol. 2011;117(4):777-87.
- Edelman AB, Gallo MF, Jensen JT, et al. Continuous or extended cycle vs. cyclic use of combined oral contraceptives for contraception. Cochrane Database Syst Rev. 2005 (3):CD004695.
- Mansour D, Korver T, Marintcheva-Petrova M, Fraser IS. The effects of Implanon on menstrual bleeding patterns. Eur J Contracept Reprod Health Care. 2008;13 Suppl 1:S13-28.
- Abdel-Aleem H, d’Arcangues C, Vogelsong K, Gulmezoglu AM.Treatment of vaginal bleeding irregularities induced by progestin only contraceptives. Cochrane Database Syst Rev. 2007 (2):CD003449.
- Mansour D, Bahamondes L, Critchley H, et al. The management of unacceptable bleeding patterns in etonogestrel-releasing contraceptive implant users. Contraception. 2011;83(3):202-10.
- Farley TM, Rosenberg MJ, Rowe PJ, et al. Intrauterine devices and pelvic inflammatory disease: an international perspective. Lancet.1992;339(8796):785-8.
- Grimes D. Intrauterine device and upper-genital-tract infection. Lancet.2000; 356:1013-9.
- World Health Organization. Medical eligibility criteria for contraceptiveuse 4th edition. Geneva: WHO, 2010.
- Hobbs MK, Taft AJ, Amir LH, et al. Pharmacy access to the emergencycontraceptive pill: a national survey of a random sample of Australianwomen. Contraception. 2011;83(2):151-8.
- Noe G, Croxatto HB, Salvatierra AM, et al. Contraceptive efficacy of emergency contraception with levonorgestrel given before or after ovulation. Contraception. 2010;81(5):414-20.
- World Health Organization. Factsheet on the safety of levonorgestrel alone emergency contraceptive pills (LNG ECPs). [cited 2012 April26]:[about 3 p.]. Available from: http://whqlibdoc.who.int/hq/2010/WHO_RHR_HRP_10.06_eng.pdf
- Piaggio G, Kapp N, von Hertzen H. Effect on pregnancy rates ofthe delay in the administration of levonorgestrel for emergency contraception: a combined analysis of four WHO trials.Contraception. 2011;84(1):35-9.
- Glasier AF, Cameron ST, Fine PM, et al. Ulipristal acetate versus levonorgestrel for emergency contraception: a randomised noninferiority trial and meta-analysis. Lancet. 2010;375:555-62.






Leave a Reply