Improving women’s health in Asia Pacific – how can RANZCOG best contribute?
I would like to begin this article with a premise – some of you may consider this a judgmental statement – and ask you to consider its veracity as objectively as you can: that the contribution of RANZCOG, and of the RACOG and RNZCOG before it, to the advancement of women’s health outside of Australia and New Zealand has been modest. What is more, RANZCOG’s level of contribution in such spheres potentially could be expanded, if we take comparable contributions of larger ‘sister’ Colleges such as RCOG (UK), ACOG (USA), and SOGC (Canada).
It is certainly true that over the last 30–40 years many individual Fellows, Associates and Trainees have contributed hugely to improving women’s health beyond Australia and New Zealand, especially in the South Pacific and in Southeast Asia. Over the same time period, our College’s contribution has tended to be relatively unstructured, at times inconsistent, and in some cases limited in substance. In part, the relative youth of our College is certainly a consideration. On another level, I have sometimes wondered whether our national psyches contain a touch of smugness and introspection at times – something of the ‘lucky country’ syndrome on both sides of the Tasman – might be a contributory factor.
Despite these personal observations, it is clear that RANZCOG is maturing in an organisational sense and I commonly hear of, and see, many Fellows and Trainees wanting to contribute to a College that seeks to help the women of our region. In my current roles, I also see more planning, strategy and intent emerging from within the College. In this vein, I would like to look at where the challenges lie and then comment on how RANZCOG and how we as Fellows, Associates and Trainees can contribute best over the coming decades.
The biggest challenges
Our ‘backyard’ consists of the island nations of the South Pacific and the numerous countries of Southeast Asia. The South Pacific countries can all be considered as low-income nations populations vary from little more than a thousand people, for instance in Niue, to over seven million in Papua New Guinea (PNG). The island nations are scattered over a truly huge part of the world’s surface. Southeast Asia, on the other hand, has many low-income nations although there are several undoubted exceptions. Populations in the low-income countries are, in the most, extremely large – Indonesia being a prime example with a population of well over 200 million people.
Low income, for any country anywhere in the world, brings the inevitable challenges to health of poverty and lack of adequate infrastructure – sanitation, water, health facilities, and information technology. In the Pacific and Southeast Asia the key tyrannies are broader still and include:
- poverty;
- inadequate and unreliable infrastructure;
- burgeoning populations and often high fecundity rates;
- political instability (and, in some instances, corruption); and
- shortfalls in health facilities, equipment and supplies and trained health workers.
Clearly, such pervasive factors all negatively impact on the provision of even vaguely adequate health services but, in addition, several factors dramatically compound the problems facing women: low education levels – both absolute and in comparison to men – and low social/societal status, with all the extremely destructive corollaries of oppression, exploitation and violence against women.
As doctors, understandably, we tend to focus on the medical means of addressing inequities in health – this is the approach with which we tend to be most familiar. Yet progress on the fundamental issues of education and status of women could potentially make a much greater impact on the health of women and children in our region.
Difficulties for women and their families don’t stop there, we need to add several relatively modern-day phenomena:
-
- The loss of skilled health workers and administrators (brain drain) to high-income, developed nations.
- Poignantly, this of course includes migration to Australia and New Zealand.
- The rise of chronic, non-infectious diseases; diseases of the West, if you will.
- The complexities of reliance on international aid and the negative consequences of short-term, unsustainable aid projects.
If we are to distil this into medical issues for women and children in
the Pacific and Southeast Asia, we see:
- high perinatal morbidity and mortality rates;
- high maternal morbidity and mortality rates – currently many of the data available on such matters are estimates at best as data-collection systems are rudimentary or non-existent in some nations – PNG has maternal mortality rates of in the order of 733 per 100 000 live births1, placing it in the group of countries with the highest rates in the world;
- high fecundity rates, low contraception rates, high rates of unsafe abortion;
- endemic violence against women and children, family and partner violence included;
- high rates of infertility;
- increasing prevalence of HIV;
- high rates of certain malignancies – as an unenviable example, Fiji has an extremely high incidence of carcinoma of the cervix(51 per 100 000 women, compared to eight per 100 000 in New Zealand2), but lacks a comprehensive screening program and has no radiation facilities for treatment of women; and
- escalating rates of chronic, non-infectious diseases, including diabetes, hypertension, chronic airways disease and joint disease.
Putting matters simply and somewhat brutally, in 2013, in many nations of the Pacific and Southeast Asia, life for women and their children is still extraordinarily arduous and hazardous. The burden of disease – in every sense of the word – is extremely heavy.

Sustainable, scalable improvements in low-resource countries’ healthcare systems are the key to happy outcomes for women and babies.
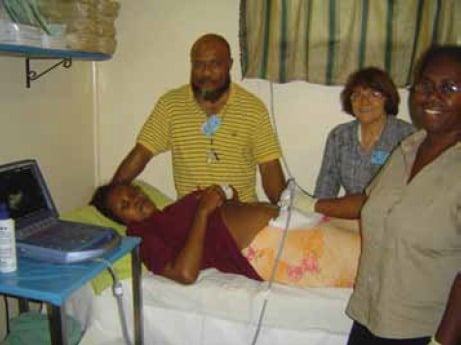
RANZCOG-supported ultrasound training in Honiara.
RANZCOG’s role
Where do we as a College, and as individuals, even begin to start if we are to make a difference? What are we doing now, and what can and should we be doing? RANZCOG, both in its own right and in association with charitable Trusts and Societies, is doing many things, including:
- training and education programs for doctors, midwives and nurses in the South Pacific;
- administrative support for the Pacific Society of Reproductive Health and for the Brian Spurrett Foundation; and
- coordination and administration of a CPD program for RANZCOG Associates working in the Pacific.
Some Fellows, Associates and Trainees contribute huge amounts of time and energy on a voluntary basis to a range of projects and initiatives in the region. As a substantial and worthy medical College, there is, I believe, opportunity for us to collectively increase our levels of activity in furthering women’s health in our wider region. If we are to meaningfully contribute we need to:
- Develop a clear and strategic approach.
- Work with the people and governments of the countries we are endeavouring to support, and with all relevant agencies.
- Working with other medical Colleges will also make sense in many instances.
- Focus on capacity building and sustainability of whatever we help to build.
- Build on our strengths, for example:
- in education, training and support of health professionals working in the Pacific and Southeast Asia;
- in coordination and facilitation of volunteers, locums and donations; and
- in advocacy on Women’s Health and women’s rights in the Pacific and Asia, in Australia and New Zealand, and at international forums, including FIGO.
In everything we do, we must work with our neighbours to build culturally sound, sustainable improvements in health systems to benefit women’s health. I believe there is great potential for our to College further advance its level of endeavour in this arena. We can take this opportunity to advocate for improvements in the social status, education and health of women in the Pacific and in Southeast Asia. We may be pleasantly surprised at how much notice is taken of what we have to say, by the public and by agencies and governments.
References
- Ministerial Taskforce on Maternal Health in Papua New Guinea –
Report May 2009. National Dept of Health, Papua New Guinea –
UNFPA. - Sunia Foliaki et al. Cancer Incidence in Four Pacific Countries: Tonga, Fiji Islands, Cook Islands and Niue. Pacific Health Dialogue March
2011, Vol. 17, No. 1.






Leave a Reply