Working in some of the most deprived regions of the world, Médecins Sans Frontières continues to witness the large scale of maternal mortality and strives to improve its delivery of care to reduce it.
This magazine’s last issue (O&G Magazine Vol 15 No 1) focused on maternal death, detailing the key causes of mortality for mothers – postpartum haemorrhage (PPH), sepsis and hypertensive disorders – and how, even in the developed world, their risk cannot be overstated.
Every year around 287 000 women globally die from complications during pregnancy and childbirth – 99 per cent in developing countries – and most of these deaths are avoidable. Nearly a third of developing-world mothers still receive no skilled care during birth or immediately after delivery.1 Annually, three million babies lose their lives in their first four weeks, again 99 per cent of them in developing countries.2 Mothers, and babies, often die at home, having never reached a health facility – deaths that may never be recorded. Thus the maternal mortality ratio (MMR; maternal deaths/100 000 live births) may be highly underestimated.
International humanitarian medical aid organisation Médecins Sans Frontières works in some of the most deprived contexts for women worldwide. It provides emergency obstetric and neonatal care in the highest mortality countries, as well as during natural disasters and conflict situations.
This article shares some of the numerous challenges to delivering that care. I am an obstetrician who has spent four years working in the field to improve the odds of survival for women in countries such as Democratic Republic of Congo, Liberia and Pakistan. Today, I am based in Sydney, and work as a medical advisor within Médecins Sans Frontières’ medical department.
The disparity in terms of health indicators between developed and developing countries is greater for maternal mortality than for any other.3 According to the World Bank, the MMR is highest in Chad (1100), followed by Somalia, Sierra Leone and Central African Republic.1 Nigeria has an MMR of 630. However, a retrospective (1990–1999) population-based study of 171 621 deliveries in Kano state in northern Nigeria estimates an MMR of 24204 – more than three times the official country average – and thus highlights the problem of underreporting and regional variation.
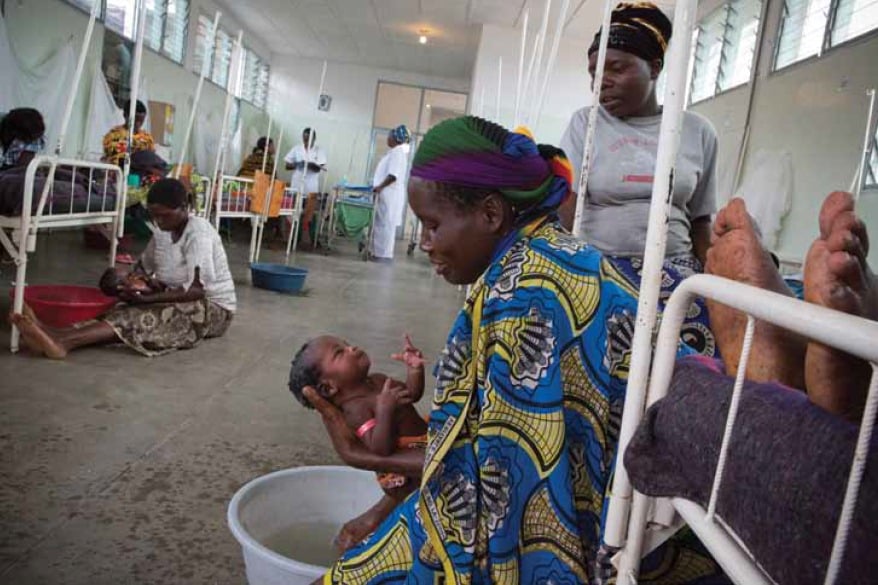
Mothers wash their newborns in one of three post-natal wards in the emergency centre for gynecological and obstetric care managed by Médecins Sans Frontières’ since 2006 in Kabezi district, Burundi. The organisation has worked in Burundi since 1992. © Sarah Elliott 2012.
Australia has an MMR of 8.4 and New Zealand, 17.8.1 A big hospital in Sydney, averaging 5000 births a year, may experience no maternal deaths in a year. Médecins Sans Frontières’ project in Jigawa State, Nigeria, neighbour to the aforementioned Kano, similarly handled just over 5000 deliveries in 2012 – and recorded 80 maternal deaths. Yet the MMR of 2420 in Kano indicates this may be only 20 per cent of the likely maternal deaths in the catchment population. We may be seeing just the tip of the iceberg.
So why is mortality so high and what are the challenges to combating it?
Apart from a small percentage of women with established high-risk pregnancies (previous caesarean section or previous pre-eclampsia for example), most life-threatening obstetric complications are unpredictable and arise during labour or 24-hours postpartum. In many places where we work, where women are usually not referred early or where travel can mean significant delays, these complications present at the severest end of their spectrum. Eclampsia complicated by pulmonary oedema or stroke; severe anaemia (Hb <2 gr/dl) after placental abruption or postpartum haemorrhage (PPH); disseminated intravascular coagulation; and ruptured bladder and uterus after obstructed labour are some of the complications that an obstetrician may have rarely faced in a developed country hospital. Such complications increase the complexity of diagnosis and appropriate treatment.
Most maternal deaths in Médecins Sans Frontières’ facilities occur within 24 hours of arrival. The biggest challenge for an obstetrician is to provide prompt, skilled obstetric care knowing that death will often be unavoidable. Yet nothing is more rewarding than to find that all the obstetric knowledge acquired over long years was useful to save a woman’s life and benefit her whole family’s future. The effect of a mother’s death can have a highly fatal impact on all her young children: in the neonatal period mortality risk increases nine-fold without a mother; in children aged two to five months, this can increase up to 25 times.5
Women present late for many reasons, particularly isolation. Transport can be expensive, or non-existent. Roads may be cut or unsafe for travel. Lack of health facilities within reach compounds this. No woman should have to travel more than two to three hours to reach emergency obstetric care; in the case of PPH if she had to travel that far, she would be lucky to survive.6
Maternity waiting homes are one way of overcoming the isolation. In Médecins Sans Frontières’ projects in countries such as Sierra Leone, Democratic Republic of Congo, and the Autonomous Region of Bougainville in Papua New Guinea, women are encouraged to admit to a waiting home at the end of the third trimester. Here they are monitored with regular health checks and midwife visits, and nourished until delivery. Uptake is limited, however, by a woman’s circumstances at home. She may be the main caregiver to multiple children, if not also a breadwinner, and unable to be absent.
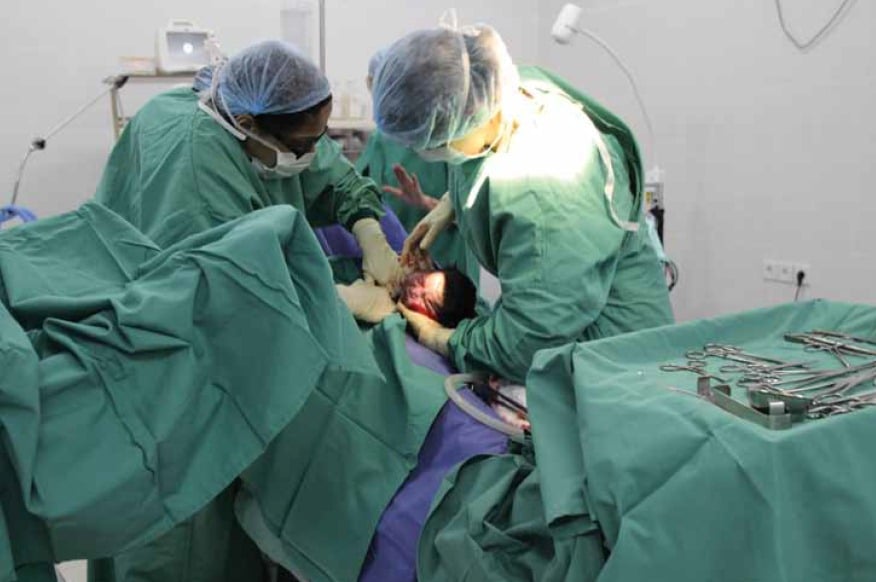
The author and team conducting a caesarean section for a woman with post-term pregnancy. Médecins Sans Frontières opened a private, secondary hospital in May 2011 in Peshawar, Khyber Pakhtunkhwa (KPK) province, Pakistan, providing free-of-charge, specialised emergency O and G care. © P.K. Lee 2011.
Multiple factors also weigh in at the time of delivery. The World Health Organisation (WHO) considers caesarean section rates of five to 15 per cent the optimal range for targeted provision of this life-saving intervention for mother and infant.7 However, caesarean section in a resource-limited setting has to be carefully considered due to the implication for future pregnancies. In places characterised by very high fertility rates, performing a caesarean section for fetal life-saving purposes might expose the woman to a higher risk of major obstetrical complications in subsequent pregnancies, owing to scarred uterus (including ruptured uterus, placenta praevia and accretism). Also, political or economic developments may make surgery unavailable the next time, whether from the national health service or an international organisation. So, although the decision whether to have a caesarean section ultimately resides with the mother, our medical guidance must reflect a range of factors that may not exist in a higher-resource context.
Médecins Sans Frontières’ strategy is based on WHO recommendations: to establish an effective referral network between basic emergency obstetric and neonatal centres (BEmONCs), where normal deliveries take place under midwives’ supervision, and comprehensive centres (CEmONCs) where surgical procedures and safe blood transfusion are available around the clock for obstetric complications. Through this strategy, mortality has been shown to decrease. In Bo district, in southern Sierra Leone in West Africa, where Médecins Sans Frontières has been present since 2008, maternal mortality today is 351,which is 61 per cent lower than the official country-wide rate of 890 per 100 000 live births. In a similar project in Burundi, in Kabezi district, the district MMR is 74 per cent lower than Burundi’s national average.8
Emergency obstetric care, access to safe abortion and family planning are identified as the most achievable, cost-effective strategies to reduce MMR in resource-poor settings.9 Médecins Sans Frontières offers all these services, but there are still major challenges to making the latter two routinely available in all projects.
Another ongoing obstacle is the lack of specialised human resources to deliver our required level of obstetric care. This lack is even more pronounced for contexts such as Pakistan and Yemen, which necessitate female obstetricians. This cultural constraint is understood and accepted, but puts a greater pressure on Médecins Sans Frontières’ recruitment needs.
The provision of emergency obstetric care is at the forefront of Médecins Sans Frontières’ work in sexual and reproductive health. The organisation will continue to expand its emergency obstetric and neonatal care programs to contribute to the survival of women, and their babies, at the most vulnerable time of their lives. The lives of women must stay high on the agenda for all health providers and political players to significantly reduce the number of avoidable deaths in the future.
To find out more about working with Médecins Sans Frontières as an obstetrician/gynaecologist, please go: to www.msf.org.au/join-our-team.
References
- World Health Organization, UNICEF, and The World Bank Estimate. Trends in maternal mortality: 1990 to 2010. 2012.
- Oestergaard MZ, Inoue M, Yoshida S, Mahanani WR, Gore FM, et al. Neonatal Mortality Levels for 193 Countries in 2009 with Trends since 1990: A Systematic Analysis of Progress, Projections, and Priorities. 2011. PLoS Med 8(8): e1001080. doi:10.1371/journal. pmed.1001080.
- Ujah IA, Aisien OA, Mutihir JUT, Vanderjagt DJ, Glew RH, Uguru VE. Factors contributing to maternal mortality in north-central Nigeria: a seventeen-year review. Afr J Reprod Health. 2005 Dec;9(3):27-40.
- Doctor HV, Findley, SE, Afenyadu, GY. Estimating Maternal
Mortality Level in Rural Northern Nigeria by the Sisterhood Method. International Journal of Population Research. 2012 (2012). 5 p. doi:10.1155/2012/464657. IJPR ID 464657. - Ronsmans C, Chowdhury MW, Dasgupta SK, Ahmed A, Koblinsky M. Effect of parent’s death on child survival in rural Bangladesh: a cohort study. Lancet. 2010;375:2024–31.
- World Health Organization. Monitoring emergency obstetric care. A handbook. 2009:14-16.
- World Health Organization. Appropriate technology for birth. Lancet. 1985 Aug 24;2(8452):436-7.
- Médecins Sans Frontières. Safe Delivery: reducing maternal mortality in Sierra Leone and Burundi. 2012:5.
- Prata N, Sreenivas A, Vahidnia F, Potts M. Saving maternal lives
in resource-poor settings: facing reality. Health Policy. 2009
Feb;89(2):131-48.






Leave a Reply