Assessment of the woman referred to the general gynaecology clinic for management of prolapse – a guide for Trainees.
Depending on the patient population, somewhere between ten and 30 per cent of women will report symptoms suggestive of pelvic organ prolapse (POP) at some time in their lives. Although this is usually a benign condition, prolapse can have a marked effect on a woman’s quality of life (QoL), potentially interfering with work, leisure activities, urinary and anorectal function, and sexual intimacy. For this reason, it is important that any woman who is referred for assessment of a possible prolapse is given a careful and thorough history and examination, to provide her with the best possible information about her condition and options for management.
Taking a relevant history
In addition to reading the referral letter, it is important to spend time listening to the woman and the issues she describes. Occasionally, completely asymptomatic women will be referred with ‘prolapse’ after examination for some other purpose (typically a Pap smear) revealed findings that concerned the family doctor. In most cases, though, women will give a history that suggests POP may be a problem. One of the lessons of POP assessment is that the symptoms a woman reports may bear little relation to the clinical findings and extent of any POP present. Some women report very bothersome symptoms, yet have a minimal degree of POP, and conversely other women seem to be little troubled, yet have impressive clinical findings.
Although assessment of the signs of POP – in particular, bulging or protrusion from the vagina – is important, it is vital to consider symptoms in context with the woman’s overall functional capacity and wellbeing, including urinary and bowel problems, and sexual function and satisfaction. Because such symptoms can be embarrassing to admit, if the woman doesn’t volunteer information, it must be specifically sought in a tactful and sensitive manner.
Ask the woman to describe the symptoms as she experiences them. This will typically be a vaginal bulge, but it may not be present all the time. Straining, prolonged standing or walking, and worsening symptoms at the end of the day are common, as is reduction of the bulge and abatement of symptoms when recumbent. The presence of a permanent bulge may suggest an advanced stage of POP (see Figure 1). In association with bulging, women may describe a ‘bearing down’ or dragging sensation, and sometimes low back pain. With severe prolapse, there may be ulceration (commonly seen with procidentia), but this should always provoke further assessment to rule out pre- or frankly malignant disease.
Continence and urinary symptoms
POP and problems with urinary continence commonly occur together and these may not be volunteered. Ask about the symptoms of urge incontinence, incomplete emptying of the bladder and bladder overactivity. These can occur with urinary retention and rapid bladder refilling and irritation. Also, specifically ask about involuntary loss of urine with straining, such as jumping and coughing or sneezing. When a large degree of anterior vaginal wall prolapse is present, this may lead to kinking of the urethra, with the potential for voiding dysfunction and episodes of retention or difficulty in initiating micturition. Some women will provide a history of recurrent urinary infections. Incontinence with intercourse may also be a significant symptom.
Bowel symptoms
Where there is a degree of posterior compartment prolapse, women may report difficulty in emptying the bowel. This may be the result of the full rectum bulging forward rather than out through the anus with straining. In some cases, women will need to put their fingers in the vagina to try to assist defaecation. This may lead to chronic incomplete rectal emptying with resulting anal overflow incontinence and frequency. The dissipation of expulsive forces during attempted emptying of the rectum with the rectum protruding into the vagina is termed a ‘defaecatory disorder.’ These problems can be acutely embarrassing and require privacy and sympathetic questioning to fully evaluate, for obvious reasons.

Figure 1. Sometimes the diagnosis of POP is obvious, as in this case of procidentia. Image courtesy of Dr David Knight.
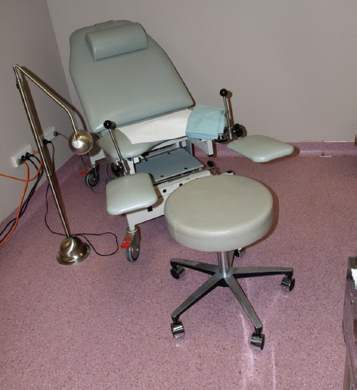
Figure 2. A comfortable couch that ensures the woman is not lying fully recumbent, with access to the perineum, is important for accurate and thorough assessment of POP.
Prolapse and sexual function
Another issue women may be reluctant to bring up is sexual difficulty. This is commonly reported by women with prolapse, for various reasons. The vaginal bulge of POP may be a hindrance during intercourse and may be uncomfortable, especially if there is associated vaginal and vulval atrophy. Damage to the levator muscles, including avulsions, often widen the genital hiatus and may be associated with reduced sensation and satisfaction, even reduced capacity for orgasm. Women are also often sensitive about their appearance and may wish to avoid sexual intimacy for these reasons. All of these factors can impact quite severely on body image, self-esteem and confidence, affecting relationships adversely.
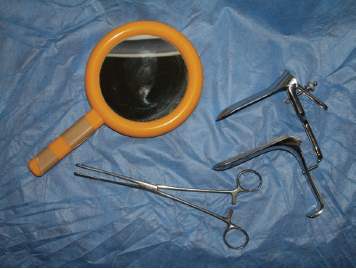
Figure 3. The basic equipment required for assessment of POP.
The broader history
Once a focused and detailed history of prolapse and associated pelvic symptoms has been taken, a broader history should be sought. In a younger woman, whose family is not complete, it is important to have a clear idea about plans for future childbearing.
A detailed obstetric history should be taken, including the number of pregnancies and deliveries, mode of delivery, birthweights and complications. POP is much more common in parous women than nulligravid women and each additional delivery increases the risk of prolapse. Other strong risk factors include: the woman’s age and, particularly, the time since menopause (particularly for women with an early menopause); overweight and obesity; previous surgical procedures for POP; and a history of POP in first-degree female relatives.
Box 1. Commonly-used systems for the documentation of examination findings in POP
Pelvic Organ Prolapse Quantification (POP-Q) system
This system uses a series of standardised points and measurements to provide very formal measurement of prolapse, allowing a staging. There are multiple resources available to help in familiarising yourself with this system, including some excellent tutorials on YouTube™. The points (A, B, C, and D) as well as the measurements are illustrated in the article on p49.
Baden-Walker system
This is a more descriptive system, not requiring formal measurement with rulers.
| Grade | Posterior urethral descent, lowest part other sites |
| 0 | Normal position for each respective site |
| 1 | Descent halfway to the hymen |
| 2 | Descent to the hymen |
| 3 | Descent halfway past the hymen |
| 4 | Maximum possible descent for each site |
Shaw system
The Shaw system is another descriptive system.
| Anterior wall | Upper 2/3 cystocele | Lower 1/3urethrocele | |
| Posterior wall | Upper 1/3 enterocele |
Middle 1/3 rectocele | Lower 1/3 deficient perineum |
| Uterine prolapse |
|||
| Grade 0: | Normal position | ||
| Grade 1: | Descent into vagina, not reaching introitus |
||
| Grade 2: | Descent to the introitus | ||
| Grade 3 | Descent past the introitus | ||
| Grade 4: | Procidentia | ||
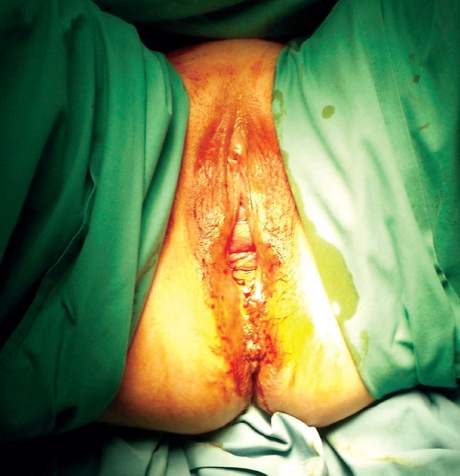
Figure 4. Wide and open genital hiatus, with anterior and posterior compartment prolapse, in a patient about to undergo pelvic floor reconstruction.
Previous treatment for POP should be enquired about, such as surgery or use of pessaries. If pessaries have been used, how well did they control the symptoms and did they precipitate other problems, such as urinary problems or defaecatory dysfunction? If surgery has been performed, what exactly was done, and what were the results? Was there a short- or long-term benefit? These are important questions, since previous use of mid-urethral tapes, sacrospinous suspensions and colpopexy procedures have been associated with a risk of later anterior compartment prolapse. Similarly, colposuspension procedures can be associated with development of enterocoele.
A general gynaecological history is important, since some women may have other problems, such as menstrual disorders, that also require assessment and management. Other significant issues include previous hysterectomy and the use of hormone replacement therapy.
Many other health problems will impact on either the woman’s overall QoL or her suitability for various treatments. Make sure a thorough drug history is taken that may be clinically relevant, such as anticholinergics, diuretics and drugs effecting coagulation. Also, women who smoke should be encouraged to quit, and any medical condition stabilised.
The management of any POP must be undertaken within the overall context of a woman’s life and responsibilities. It is important to take a social history, as women need care and support in the post-operative period and may face difficulties in caring for partners or relatives if they undergo surgery, including the need for heaving lifting. Advice should be given about the need to abstain from intercourse after vaginal surgery until the post-operative visit. Make sure you understand a woman’s occupation and its demands, as this can affect the time required away from work. POP can have a significant effect on QoL, and a formal assessment can be performed using a validated questionnaire, such as that of Digesu and colleagues (see further resources at the end of this article).
Examination
Conducting a useful clinical examination requires some basic items of equipment. Perhaps most importantly, a suitable examination couch is essential (see Figure 2). This should allow the clinician good access to the perineum. A couple of simple items are all that are required to complete the examination and it is useful to use a hand mirror, so that women can see what the findings are and have them explained (Figure 3).
Assessment of the woman’s general state of health is important and will include weight, body mass index and blood pressure, as well as assessment of any varicose veins or hypermobile joints, since these can be markers of a tendency to connective tissue laxity which predisposes to POP and, importantly, to recurrence after surgical repair.
On examination of the abdomen, inspect for incisions of previous surgery (which may be associated with intra-abdominal adhesions affecting subsequent surgical approaches) and to exclude masses or ascites (which are embarrassing to discover later). The presence of umbilical or other herniae can, again, indicate underlying connective tissue weakness and may require concomitant surgical correction.
On inspection of the vulva, note the presence of any atrophy and whether there is any ulceration of prolapsed tissues that may necessitate therapy with oestrogens, especially if surgery is planned. The normal genital hiatus is closed, with an area of only a few square centimetres, and an open hiatus with the vaginal walls visible indicates probable damage to the levator muscles, usually an avulsion injury (see Figure 4). Another important indicator of levator avulsions is midline asymmetry, sometimes apparent with straining.
With the woman reclining, but not lying flat, ask her to strain or bear down. If there is a bulge from the vagina, note whether the pattern of rugae (formed by muscle and connective tissue deep to the skin) is present, which indicates an intact fascial layer in the midline and a probable lateral defect, or absent, suggesting a midline defect with only skin and attenuated connective tissue present. In some cases, straining or coughing will precipitate stress urinary loss or rectal prolapse, both of which are important findings.
Examination with a bivalve speculum allows assessment of the cervix (including a Pap smear, if appropriate), but not prolapse. The use of either a Sims’ speculum or a disassembled bivalve speculum is required to carefully assess the anterior and posterior compartments and to assess the supports of the cervix or the vault if there has been a previous hysterectomy. It is common to require Rampley’s sponge-holding forceps to aid in support of the vaginal walls, as this can obscure the view. At the completion of the speculum examination, perform a bimanual examination to check the uterine size and mobility, as well as to exclude unsuspected adnexal pathology, such as ovarian tumours. This also allows an assessment of vaginal muscle tone. Rectal examination is not usually required unless specifically indicated, but may distinguish rectocoele from enterocoele. Make sure you ask the woman to direct your attention to any other findings she has noted, that you haven’t discovered or that she wants to draw your attention to.
Quantifying and documenting the findings
As well as recording detailed notes about the findings, it is important to standardise descriptions, particularly if referral for a subspecialist opinion is being contemplated. Rather than vague descriptions (moderate prolapse) time spent using a formal descriptive system such as the POP-Q, Baden-Walker or Shaw systems (depending on local custom) is time well spent. These systems are briefly described in Box 1. It is beyond the scope of this article to detail these various systems.
Conclusion
Take a thorough history and perform a careful physical examination of women who are referred for assessment of prolapse. Make sure you understand each woman’s life circumstances and responsibilities, as these can have a very important influence on the treatment you initiate. Examination should be carried out with dignity and care, using some basic tools that aid in the accurate evaluation of anatomical and functional defects. Encourage the woman to view your examination and its findings with a hand mirror and explain what you find as you go along. Use a standardised assessment system to document your findings and make sure you explain everything in understandable terms. Good luck.
Further reading
Digesu G, Khullar, Cardozo L, et al. P-QOL: a validated questionnaire to assess the symptoms and quality of life of women with urogenital prolapse. Int Urogynecol J. 2005; 16: 176-81.
Lowenstein L, Gamble T, Sanses T, et al. Changes in sexual function after treatment for prolapse are related to the improvement in body image perception. J Sexual Med. 2010; 7: 1023-8.








Leave a Reply