Procidentia refers to the complete prolapse beyond the level of the hymen distally so the uterus (or vaginal vault if uterus is absent) is permanently protruding out of the vagina.
Pelvic organ prolapse (POP) is defined as the symptomatic descent of one or more of: the anterior vaginal wall, the posterior vaginal wall, and the apex of the vagina (cervix/uterus) or vault (cuff) after hysterectomy, according to the International Continence Society (ICS) definition and standardisation nomenclature 2009. In practical terms, it refers to a caudal displacement of the female pelvic organs as a result of weakening of supporting tissues of the vagina and uterus, resulting in extrusion of the pelvic organs to the genital hiatus. There have been a number of methods used to quantify the degree of severity of POP, but only one system has been validated for inter and intra-observer reproducibility, which is the POP quantification (POP-Q) ICS quantification system.
Scandinavian studies involving asymptomatic women invited for assessment reported that 55 per cent of women aged from 40–49 years had, on examination, POP of greater than grade two in at least one compartment.1 Of women aged between 50 and 79 years in the Women’s Health Initiative (WHI) study, 41 per cent had POP, with 34 per cent having a cystocele, 19 per cent a rectocele and 12 per cent found to have uterine prolapse. Studies from the USA, looking at operations for POP, suggest that one in nine women will require an operation by the age of 80 years. However, since many women do not seek medical assessment, it is very likely that the burden of disease in the population is underestimated.
Important risk factors include parity, since the incidence of POP increases with increasing parity: up to 80 per cent of women who have had four or more vaginal deliveries will have POP.1 In those women who were able to activate pelvic floor muscles sufficiently, this incidence was reduced by nearly 50 per cent. Use of forceps for delivery also increases the risk significantly, with other less-important factors being the duration of labour, use of episiotomy, birthweight, and previous hysterectomy. There are racial variations, with studies from the USA reporting that Asian women have a higher incidence and African women have a lower incidence.3
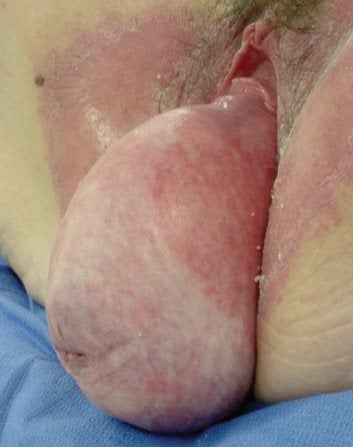
Procidentia is easy to identify.
The support mechanisms of the uterus and vagina are still not fully understood, but relate to a complex interaction of fascial integrity and ligamentous connections to bony structures. Endopelvic fascia surrounds the vagina, but controversy still exists as to whether there are distinct layers or spaces or whether the vaginal mucosa and muscularis merge or interdigitate with collagen and elastin submucosally. This sock-like tissue then coalesces with the cervical cuff cranially to integrate with uterosacral and cardinal ligaments as well as laterally to the underlying levator ani muscle attaching to the arcuate line of the levator fasciae pelvis, which runs from the ischial spine to the pubic insertion of puborectalis. Caudally the fascia connects to the perineal membrane and perineal musculature. The support of the urogenital organs have been segregated into three different levels: Level 1 being the uterosacral/cardinal complex cranially, level 2 the endopelvic fascia surrounding the upper two-thirds of the vagina and level 3 the lower third of the vagina as it attaches to the levator ani and perineal membrane.4 In reality, this is an integral system of support with multiple potential areas for disruption or weakness.5 Underlying this is a secondary support mechanism of the levator ani muscle, and in particular the puborectalis ‘sling’ that acts to support the vagina at the level of the levator hiatus, and the disruption of which is common after vaginal childbirth6, predisposing to POP in later life.7
A careful history of urinary, bowel and coital symptoms is important to optimise patient centred outcomes. There are a number of validated questionnaires for this, for example being the Australian pelvic floor questionnaire.8 Examination needs to quantify the POP and any other associated urogenital weakness. The investigations required with procidentia are few, but renal ultrasonography and mid-stream urinalysis may be important, owing to potential for kinking of the ureters leading with consequent hydronephrosis and urine stasis due to incomplete emptying. In addition, some authors have suggested urodynamic investigations prior to surgery to help identify occult stress urinary incontinence and to attempt to predict those women with underlying voiding dysfunction. Assessment of POP is largely clinical, augmented by imaging modalities such as ultrasonography and MRI. For practical purposes, although such investigations may be useful for a research aspects, they are not usually warranted.
Management can be non-surgical, with the use of pessaries, although successful long term treatment may be difficult. The use of pessaries is beyond the scope of this article. Whatever treatment is chosen, pelvic floor rehabilitation with continence nurses or physiotherapists trained in women’s pelvic health, is an important adjunct to obtaining a successful long-term outcome. Often, women with procidentia have poor coordination of pelvic muscle relaxation and contraction, associated bowel dysfunction, and underlying urinary incontinence and this complex range of pathology should be managed as a ‘global’ pelvic disorder. Weight loss, smoking reduction and improvement of bowel habit, although not proven to improve outcome, are important to address prior to surgery.
Surgical options: to conserve or not?
This is a controversial area and there is limited work to suggest uterine preservation offers any advantage. There are a plethora of operations with advocates extolling the advantages of each based on personal experience (bias) and limited cohort studies, usually retrospective. So definitive recommendations for surgery are limited to major studies as summarised in the Cochrane review. The Cochrane review of 2013 would suggest abdominal sacrocolpopexy, either by open or laparoscopic technique, may offer marginally better outcome for uterine or vault prolapse mainly in terms of vaginal length and sexual outcomes as well as recurrence rates when compared to total vaginal mesh implants. However, operating times were longer and there was a longer period before a return to work.
Surgical options for procidentia include: vaginal hysterectomy with anterior and posterior traditional colporrhaphy; or vaginal hysteropexy utilising uterosacral and cardinal ligament complex; sacrospinous fixation; or abdominal or laparoscopic hysteropexy, with or without mesh.
Surgical options for vault prolapse include: abdominal or laparoscopic sacrocolpopexy, with or without mesh; sacrospinous fixation; McCall culdoplasty; uterosacral fixation – intra- or extra-peritoneal; ileo-coccygeal fixation; or vaginal mesh colpopexy with or without fixation to sacrospinous ligament using biological or synthetic polypropylene.
Colpocleisis is a surgical option for both procidentia and vault prolapse. As in any surgery where the uterus is conserved, an endometrial assessment should be undertaken at the same time.
Evidence for synthetic mesh augmentation is present for sacrocolpopexy and vaginal mesh kits.9 With increasing concern about the complications of mesh-augmented repair vaginally, mainly as a result of vaginal contraction, pain and mesh exposure post-operatively, there has been a move back to native tissue repair. Simple vaginal hysterectomy with or without associated anterior and posterior vaginal repair is associated with relatively poor long-term outcome and logically, unless level 1 weakness is addressed at the time of surgery, simply removing the uterus unless related to elongation of the cervix makes little sense.
Sacrospinous fixation using needle holders and sutures, or reusable deployment and capture devices and disposable suture catch devices have made this procedure easier to perform. However, significant lateral dissection is required to identify the portion of the sacrospinous ligament that is safe to use, which is approximately 2cm cranial and medial to the ischial spine. Risks include deployment too deep, resulting in injury to the pudendal bundle or inferior gluteal vessels or sciatic nerve. Buttock pain can be a complication of this procedure, but with newer catch devices seems to be reduced and limited in duration. Persistent severe pain lasting more than 48 hours may require release of the sutures. Although traditionally unilateral, because of concerns of tethering and tenting of the vagina, bilateral fixation is increasingly undertaken with excellent elevation and can be done without painful tethering. Long-term outcomes suggest higher recurrence rates, compared to sacrocolpopexy, and when undertaken posteriorly can result in increased de novo anterior compartment prolapse. Anterior fixation, although technically more challenging, may improve this outcome and some centres advocate a four-point fixation, incorporating both anterior and posterior level 1 support to overcome this.
Uterosacral fixation can be undertaken at the time of hysterectomy when anatomy is easier to define or by means of plication for uterine sparing and some studies have suggested good results.10,11 For vault prolapse, intra-peritoneal fixation can be technically challenging and all of these procedures run an increased risk of ureteric injury. Extra-peritoneal fixation has also been shown to have good results and avoids entering into the abdominal cavity.12
Ileococcygeal fixation is technically easier, but results in lower success rates. The McCall, or a modified McCall procedure utilising the uterosacral ligaments, is a relatively straightforward procedure that results in good anatomical correction. Colpocleisis involves permanent closure of the denuded anterior and posterior vaginal mucosa, aiming to obliterate the vaginal cavity. It is suitable for the elderly and has relatively low morbidity.
In summary then, the optimal surgical treatment of procidentia depends on patient-focused outcomes, including desire to maintain sexual intercourse, desire to keep her uterus and the history of previous pelvic surgery. At this stage, further studies are required to clarify the best treatment for this end-stage disease.
References
- Samuelsson E, Victor A, Svardsudd K. Determinants of urinary incontinence in a population of young and middle-aged women. Acta Obstet Gynecol Scand. 2000;79(3):208-15. PubMed PMID: 10716302.
- Thakar R, Stanton S. Management of genital prolapse. BMJ. 2002;324(7348):1258-62.
- Hendrix SL, Clark A, Nygaard I, Aragaki A, Barnabei V, McTiernan A. Pelvic organ prolapse in the Women’s Health Initiative: gravity and gravidity. Am J Obstet Gynecol. 2002;186(6):1160-6.
- DeLancey JO. The Anatomy of the Pelvic Floor. Current Opinion in Obstetrics & Gynecology. 61994a. p. 313-43.
- Petros PE, Ulmsten UI. An integral theory of female urinary incontinence. Experimental and clinical considerations. Acta Obstet Gynecol Scand Suppl. 1990;153:7-31. PubMed PMID: 2093278.
- Dietz HP. Levator function before and after childbirth. ANZJOG. 2004;44(1):19-23.
- Andrew BP, Shek KL, Chantarasorn V, Dietz HP. Enlargement of the levator hiatus in female pelvic organ prolapse: cause or effect? ANZJOG.
2013;53(1):74-8. doi: 10.1111/ajo.12026. PubMed PMID: 23278472. - Baessler K, O’Neill SM, Maher CF, Battistutta D. Australian pelvic floor questionnaire: a validated interviewer-administered pelvic floor questionnaire for routine clinic and research. Int Urogynecol J Pelvic Floor Dysfunct. 2009;20(2):149-58. Epub 2008/10/30. doi: 10.1007/s00192-008-0742-4. PubMed PMID: 18958382.
- Maher CF, Feiner B, DeCuyper EM, Nichlos CJ, Hickey KV, O’Rourke P. Laparoscopic sacral colpopexy versus total vaginal mesh for vaginal vault prolapse: a randomized trial. Am J Obstet Gynecol. 2011;204(4):360 e1-7. Epub 2011/02/11. doi: 10.1016/j. ajog.2010.11.016. PubMed PMID: 21306698.
- Shull BL, Bachofen C, Coates KW, Kuehl TJ. A transvaginal approach to repair of apical and other associated sites of pelvic organ prolapse with uterosacral ligaments.[see comment]. Am J Obstet Gynecol. 2000;183(6):1365-73; discussion 73-4.
- Haylen BT, Yang V, Vu D, Tse K. Midline uterosacral plication anterior colporrhaphy combo (MUSPACC): preliminary surgical report. Int Urogynecol J. 2011;22(1):69-75. Epub 2010/08/27. doi: 10.1007/ s00192-010-1242-x. PubMed PMID: 20740357.
- Fatton B, Dwyer PL, Achtari C, Tan PK. Bilateral extraperitoneal uterosacral vaginal vault suspension: a 2-year follow-up longitudinal case series of 123 patients. Int Urogynecol J Pelvic Floor Dysfunct. 2009;20(4):427-34. Epub 2009/01/23. doi: 10.1007/s00192-008- 0791-8. PubMed PMID: 19159055.






Leave a Reply