Case report
Ms Y, a 30-year-old gravida 2 para 1 (lower segment caesarean section for failure to progress), presented to the emergency department (ED) with right iliac fossa pain, ten days of amenorrhoea and a positive beta-HCG (720IU/L). Ultrasound revealed a 17mm mass in the right adnexa and a small amount of free fluid in the pelvis. She underwent a laparoscopic right salpingectomy for an ectopic pregnancy. A moderate haemoperitoneum was noted intra-operatively.
Twenty days post salpingectomy, Ms Y presented to her GP with further right iliac fossa pain, but no PV bleeding. Her beta-HCG was 980IU/L and rose to 1200IU/L after 48 hours, upon which she was referred back to the ED. Review of histopathology from Ms Y’s recent salpingectomy confirmed a tubal gestation. Ms Y denied any sexual intercourse since discharge. Subsequent transvaginal ultrasound revealed cystic structures within her caesarean scar that were suspicious of a caesarean scar ectopic.
Ms Y was transferred to a tertiary centre for further imaging and management. A second ultrasound confirmed the diagnosis of a caesarean scar ectopic. She was treated with intravenous methotrexate upon which her beta-HCG dropped appropriately.
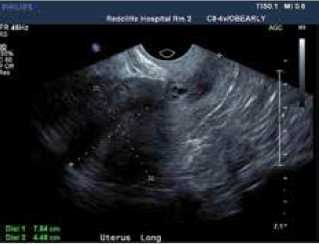
Figure 1. Ms Y’s ultrasound findings consistent with a caesarean scar ectopic.
Discussion
Ms Y presents an unusual case of a caesarean scar ectopic with uncertain aetiology. Two hypotheses have been proposed to explain her clinical course. Firstly, an early secondary abdominal pregnancy post spontaneous tubal abortion and, secondly, a heterotopic pregnancy with two ectopic gestations.
Secondary abdominal pregnancies are very uncommon.1 They have been reported following a tubal ectopic rupture, removal or abortion and, very rarely, later in pregnancy, following uterine rupture.2 It is hypothesised in this case that Ms Y’s right tubal pregnancy miscarried into the abdomen and some of this tissue implanted into her caesarean scar, resulting in the caesarean scar ectopic. No case reports of secondary abdominal pregnancies resulting in caesarean scar ectopics could be found in the literature.
Heterotopic pregnancies, where two simultaneous gestations implant at different sites, occur in one in 30 000 spontaneous pregnancies.3 This incidence is significantly increased with artificial reproductive technology (ART) to approximately two per cent of ART pregnancies.3 The most common form of a heterotopic pregnancy is with one intrauterine gestation and one extrauterine gestation (most commonly in the fallopian tube). No case reports of simultaneous tubal and caesarean scar ectopic gestations could be found in the literature.
Conclusion
The incidence of caesarean scar ectopics is increasing with rising caesarean rates. It is reported to occur in approximately one in 2000 pregnancies where the woman has had a previous caesarean section.4 There is no clear management guideline for a caesarean scar ectopic. Treatment options are aimed at minimising complications and preserving fertility: methotrexate is commonly used.5
It is not routine to re-test beta-HCG in women post laparoscopic removal of tubal ectopic pregnancies. However, with the rising incidence of heterotopic pregnancies and the risk of secondary abdominal pregnancies, one must ask whether it is wise to start doing so. A repeat beta-HCG assay could be considered in all women, particularly in women who have undergone ART or whose tubal ectopic has ruptured or aborted. Whether this should become routine is for the reader to decide.
References
- Ali R, Fitzgerald C. Omental and peritoneal secondary trophoblastic implantation – an unusual complication after IVF. Repro
BioMed. online 2006;19:776-778. - Giannopoulos T, Katesmark M. Ruptured tubal ectopic with secondary implantation in pouch of douglas. J Obstet Gynaecol. 2004;24:199-200.
- Rojansky N, Schenker J. Heterotopic pregnancy and assisted reproduction – an update. J Assist Reprod Genet.1996;13:594-601.
- Rotas M, Haberman S, Levgur M. Cesarean scar ectopic pregnancies: etiology, diagnosis and management. Obstet Gynecol. 2006;6:1373-1381.
- Litwika K, Greco E. Caesarean scar pregnancy: a review of management options. Curr Opin Obstet Gynecol. 2011;23:415-421.






Leave a Reply