Fertility and assisted reproductive technology (ART) frequently feature in the tabloid press, competing for space with the Kardashians and advertisements for breakfast television. It is a testament to the universal experience of reproduction– mixed with a good dose of pioneering medical science at the boundaries of ethics and fuelled by commercial interests – that this subject continues to dominate the headlines. This review takes a pragmatic approach to the stories that have caught the headlines in last few decades, selecting specific topics that have captured the public imagination.
The good
Louise Brown, the first live birth conceived by IVF, was born on 25 July 1978, by planned caesarean section in Oldham, UK. It will come to no surprise to anyone who has worked in the UK that she was delivered by the registrar, John Webster, who was, unfortunately, largely forgotten in the most-featured medical story of the decade. Instead, Patrick Steptoe and Robert Edwards, as the ‘fathers’ of in vitro fertilisation (IVF), dominated the front page of every regional paper, including the front covers of Life and Time magazines. Edwards was eventually awarded the 2010 Nobel Prize in Medicine for his work. Of course, this achievement was the culmination of decades of scientific discovery and multiple teams around the world were racing to publication. By the mid-70s, the Americans had been pushed out of the race and the British and Australian teams were fighting for a breakthrough. The Australian team, led by Carl Wood, had taken the lead with the publication of the first pregnancy which, unfortunately, resulted in an early miscarriage. While that crucial first live birth eluded them, Australia pioneered modern IVF.
It is not surprising that with such high stakes, the British teams managed their relationship with the media very carefully. Publications were short, directed and followed by controlled press conferences. Information surrounding the pregnancy was tightly guarded and the Brown family signed an exclusivity deal with the Daily Mail, which managed the build up to the delivery. Lesley Brown was booked into the hospital under a pseudonym and the birth was filmed by the Central Office of Information in secrecy to manage the media and competing commercial interests. In this setting, it would have been expected that such a momentous occasion would be celebrated by a landmark paper, rather than a mere Letter to the Editor. To the chagrin of the protagonists, such was the suspicion of commercial gain before scientific rigour, that the Chicago-based fertility research organisation, the Barren Foundation, cancelled their award presentation to Patrick Steptoe.
Male factor infertility remained the great challenge of assisted reproduction until the introduction of intracytoplasmic sperm injection (ICSI), a technique that evolved from subzonal insemination (SUZI). ICSI has become the face of IVF: the image of the micromanipulated oocyte at the time of sperm injection, with its subtle but unmistakable symbolism, has become the posterchild of modern reproduction. Following in the footprints of Steptoe and Edwards, this breakthrough was again announced with little more than a Short Report in the Lancet by Gianpiero Palermo from the Center for Reproductive Medicine in Brussels, headed by Paul Devroey and Andre Van Steirteghem. Reportedly, the first embryo was produced in 1990 and the first baby was born in January 1992. Embryologists have always argued that the technique evolved more by accident than design, as scientists were inadvertently entering the ooplasm during the procedure, which would certainly account for the publication delay.
The controversial
Reproduction at any cost
Assisted reproduction has the capacity to achieve conception in situations beyond natural reproduction, and this is nowhere more evident than with extreme reproductive assistance.
The oldest mother
Maria del Carmen Bousada de Lara made headlines around the world when her twins were delivered by caesarean section in Barcelona, Spain, in December 2006, one week before her 67th birthday. The case made headlines for a number of reasons: Maria had attended a fertility clinic, claiming to be 55 years of age and had sold her house to raise the reported US $59 000 to pay for fertility treatment in the US. Her family was unaware she had gone overseas for fertility treatment and publicly criticised her decision. Despite her hopes that she would live to 101, like her own mother, and be able to raise her family, she died in 2009 from gastric cancer.
Two years later, Rajo Devi became the verified oldest woman to give birth to a singleton female on 29 November 2008, though Omkari Panwar has been claimed to be the oldest mother after the birth of twins, in July 2008. As she has no birth certificate, sources have variably estimated her age between 70 and 72 at the time of the birth.
In Australia and New Zealand, fertility units set their own age limits for assisted reproduction, though most would limit treatment to the time of expected menopause. In Australia, one in four women accessing reproductive assistance are now over the age of 40. In 2013, there were 903 autologous fresh cycles in women over the age of 45, resulting in 21 pregnancies and 11 live births. Similarly, there were 575 donor cycles initiated in recipients over the age of 45, resulting in 142 pregnancies and 101 live births. Consequently, as the experience with conception in women of very advanced maternal age increases, the risks of pregnancy over the age of 45 have become more clear: not unexpectedly, maternal, fetal and neonatal morbidity increases in proportion with maternal age. Unfortunately, the absence of chronic disease, such as a pre-existing hypertensive disorder, is not predictive of a better maternal or neonatal outcome or significant morbidity. This issue was specifically addressed in RANZCOG Statement C-Obs 52, which advises that women over the age of 45 attempting conception be referred for medical review prior to conception.

Short reports in the medical literature, but major coverage in the lay press: the paradox of ART breakthroughs.
The highest number of multiple pregnancies
Nadya Suleman made headlines in 2009 with the delivery of octuplets in January. The medical board of California discovered that the pregnancy resulted from the transfer of 12 blastocysts in a fresh IVF cycle by her treating physician, whose licence was revoked in July 2011. The children were delivered by a team of 46 physicians in a remarkable feat of feto-maternal and neonatal medicine. Nadya’s story had all the makings of a headline: at first glance, a seemingly unassuming, average individual, hit by misfortune. Digging deeper, the story revealed a scandalous past, an existing family of six children, a donor conception, public funding and a high-profile medical practitioner, just waiting to be taken down. An instant celebrity was born and she featured in an estimated half million news reports, tweets and social media instances. Fortunately, the peculiarly US-based practice of multifetal transfers is now an anachronism in Australia and New Zealand.
Three-party reproduction
Advances in embryonic and genomic manipulation have paved the way not only for reproduction, but also for improvement. While no pregnancies have been reported from human nuclear genetic engineering, the UK hit world headlines by legalising three-party assisted reproduction. Seemingly speaking from the heart of IVF specialists worldwide, Lord Robert Winston declared to the House of Lords in 2015: ‘We do not try to supplant God. We try to augment his works.’
A number of mitochondrial disorders, such as the muscular dystrophies, are related to mutations in extranuclear mitochondrial DNA and are therefore almost entirely maternally inherited. Cytoplasmic transfer, supplementing the ooplasm with unaffected mitochondria, has been described and the first child born after cytoplasmic transfer in 1997. However, the effect of such procedures is limited and more advanced techniques, such as pronuclear or spindle transfer effectively relocate the nuclear material into a third-party oocyte. Legislative changes, as passed in the UK, will empower IVF clinics to create genetically engineered humans, that represents a breakthrough for families afflicted by disorders such as muscular dystrophy.
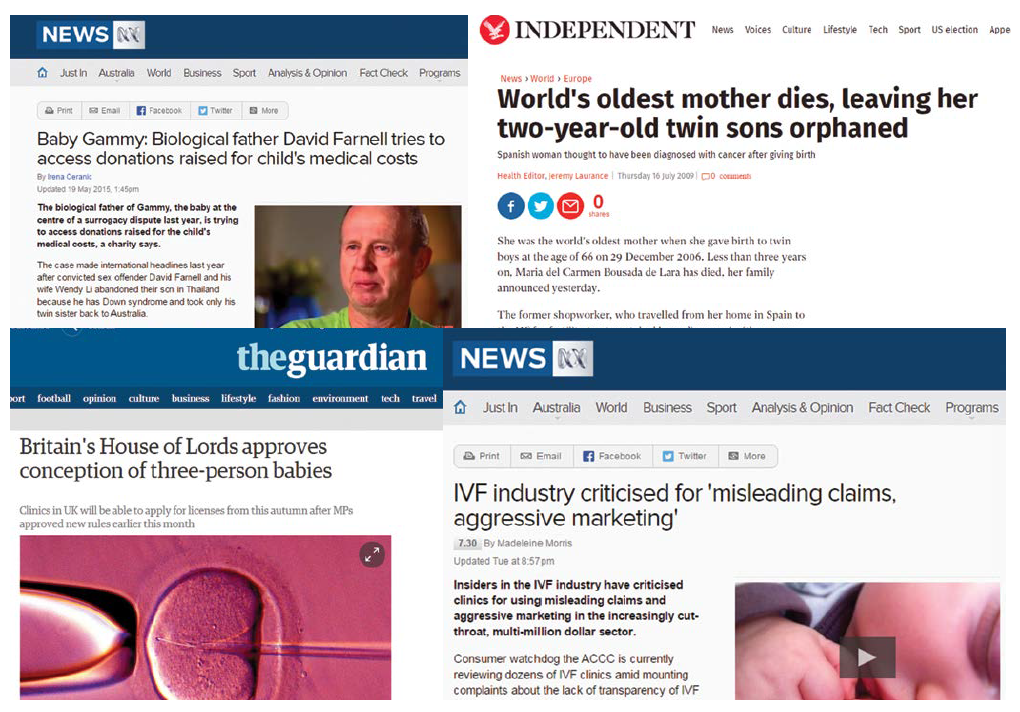
Just because you can, doesn’t mean you should: the ethical implications of scientific advances play out across the pages of the world’s media.
The ugly
Cross-border reproductive care and surrogacy
In 2014, the abandonment of baby Gammy made international headlines when a convicted sex offender, David Farnell, and his wife commissioned a surrogacy in Thailand. When Gammy was diagnosed with Down syndrome, Farnell returned only with his unaffected twin sister. The case highlighted the difficulties associated with ‘reproductive tourism’, as it became known in the popular press. The case highlighted the desperation of couples suffering from infertility and, in response, the College is developing a statement on cross-border reproductive care and surrogacy.
Transparency
In an increasingly competitive market, no radio broadcast is complete without an advertisement for yet another IVF service. It is not surprising that in such an environment, patients are looking for comparators to select their provider. At first glance, price and success rates appear to be the obvious solution. Unfortunately, the recent Australian Competition and Consumer Commission inquiry highlights the problem of presenting IVF success rates. At the most fundamental level, the definition of a pregnancy is obvious, unless you are running an IVF unit. Pregnancies have been variably defined at the point of a positive pregnancy test (usually two weeks after an egg pick up), an appropriate sequential rise in hCG, an ultrasound scan demonstrating a viable pregnancy at seven or 12 weeks, a gestation beyond 20 weeks or, most convincingly, with the delivery of a live birth. Even if a specific definition is accepted as an appropriate numerator, IVF clinics still face the challenge of how to report the pregnancy rate: should the denominator be the number of patients commencing a cycle, those progressing to an egg pick up, proceeding to transfer or the number of embryos transferred? If specialists cannot agree on uniform reporting, this issue is even more complicated for the lay public. A published pregnancy rate of 25 per cent for a blastocyst transfer in a 43-year-old is meaningless unless the patient is aware that the majority will not reach this stage and there is a high pregnancy loss thereafter. More concerning is the inevitable request to rank clinics or, worse, practitioners, which will inevitably result in those patients who most require our help to be least likely to receive treatment.
Conclusion
Looking back on almost 40 years of headlines, the profession can be filled with a sense of pride at the incredible vision, achievement and ground-breaking treatment that has occurred in this specialty. However, with achievement and controversy also comes the realisation that progress cannot proceed unmonitored and, at times, has unexpected consequences. Just like an IVF cycle.
Further reading
- Amato P, Tachibana M, Sparman M, Mitalipov S. Three-Parent IVF: Gene Replacement for the Prevention of Inherited Mitochondrial Diseases. Fertil Steril. 2014; 101(1): 31-35.
- De Kretzer D, Dennis P, Hudson B, Leeton J, Lopata A, Outch K, Talbot J, Wood C. Transfer of a human zygote. Lancet. 1973; 2(7831): 728-729.
- Devlin H. Britain’s House of Lords approvesconception of three-person babies. Guardian. 24 February 2015. Available from: www. theguardian.com/politics/2015/feb/24/uk-house-of-lords-approves-conception-of-three-person-babies .
- Irvine C. World’s oldest mothers. Telegraph. 9 December 2008. Available from: www.telegraph.co.uk/news/newstopics/howaboutthat/3689004/ Worlds-oldest-mothers.html .
- Macaldowie A, Lee E, Chambers GM. Assisted reproductive technology in Australia and New Zealand 2013. NPESU, Sydney: 2015.
- Mohajer S. Suleman’s fertility doc has licence revoked. 6 January 2011. NBC News. Available from: www.nbcnews.com/id/43241012/ns/ health-health_care/t/sulemans-fertility-doc-has-license-revoked .
- Family Criticizes 67-Year-Old Spanish Woman Who Gave Birth. 14 January 2011. Fox News. Available from: www.foxnews.com/story/2007/01/14/family-criticizes-67-year-old-spanish-woman-who-gave-birth.html .
- Palermo G, Joris H, Devroey P, Van Steirteghem AC.Pregnancies after intracytoplasmic injection of single spermatozoon into an oocyte. Lancet 1992: 340(8810): 17-18.
- Russo K. World’s Oldest Mom. 4 July 2008. ABC. Available from: http://abcnews.go.com/Health/ActiveAging/story?id=5309018 .
- Steptoe PC, Edwards RG. Birth After the Reimplantation of a Human Embryo. Lancet. 1978: 312(8085): 366.
- Woolls D. Spaniard who gave birth at 66 reported dead. 15 July 2009. Associated Press. Available from: www.nydailynews.com/news/world/spanish-woman-gave-birth-twins-66-dies-69-article-1.426204 .






Leave a Reply