During July 2016, I was privileged to be part of a team of volunteers that visited Kagando in Uganda to provide prolapse and fistula treatments and surgeries. My fellow team members were Drs Gaik Imm Tan, Barbara Hall and John Taylor and long-term urogynaecology visitors Prof Judith Goh and Dr Hannah Krause.
After an eight hour bumpy car ride from Entebbe we worked for three weeks with wonderful peers trying to alleviate some of the urogynaecological conditions faced by women so they could move towards a healthier, happier and more comfortable lifestyle.
Prolapse Camp (6–12 July 2016)
Our Prolapse Camp was held in Kagando, a town in the foothills of the Rwenzori mountains, near the border with the Democratic Republic of Congo. We arrived on the afternoon of 6 July, and wasting no time, organised our equipment. By 3pm, we were on our feet, walking to the wards to be greeted by nurse, Harriet. Harriet has worked in Kagando hospital for more than 20 years and, together with the other nursing staff, has played a pivotal role in travelling to distant villages, finding and screening women with prolapse and fistula for the camp and looking after them pre- and postoperatively.
Harriet was delighted to see us and said that she had popped in to check if we had arrived numerous times. She had more than 40 patients waiting who were starting to get worried that we were not coming. There were women sitting out on grass just outside the ward, and the hospital had set up a makeshift tent as a ward to accommodate the patients postoperatively.
We set up at the screening room where we would assess the patients to determine if they would require surgery and plan the surgery or necessary treatment. We assessed a total of 50 women within three hours, with the help of the nurses as translators. The patients included some chronic procidentias and fistulas. We even saw a child as young as eight years old.
We sat down after the screening to schedule patients for theatre and organise the operating lists for the next day. We had identified more than 40 women who required surgery, which would take place over the next five days. We got back to the guesthouse just in time for dinner, had a long-awaited shower, unpacked, organised equipment and perishables for work the next day and finally rested. The anticipation of work and settling into the new environment kept some of us awake.
The next day, we headed down to the wards by 8am to do some last-minute organisation and to see if any more patients had turned up overnight (there were none). At other times the hospital would not have to deal with such large volumes of patients over the course of a few days, so it took a while to set up the theatres and necessary instruments. We had two operating tables in the room, with a curtain separating them, but no air conditioning. We tried to maintain as sterile a setup as possible.

Ward round with prof Judith Goh, Dr Barbara Taylor and the local Ugandan team.
Once we started, we were ‘flying’, getting one patient after another on the operating table and the sole nurse anaesthetist, Richard, running anaesthetics for both operations and having to leave for a caesarean or two in between as well. Kudos to Richard, who didn’t even have time for a lunch break and didn’t complain!
We managed to complete the 11 scheduled surgeries for the day and popped by the ward to make sure the patients were all right postoperatively by 6.30pm. It was a long and rewarding day and the start of many similar days to come. Over the next five days, we operated on 46 women with prolapse. Most of them had a vaginal hysterectomy, anterior and posterior repair and a sacrospinous fixation for a stage 3 or 4 prolapse. Some of the women wanted to keep their uterus and so had hysteropexies.
It was very hot in theatre under scrubs, plastic aprons and gowns and at the end of each operation our scrubs were very wet! There were times when the electricity and water went off and we just used our battery-operated headlights to see what we were doing.
We had lunch brought down to the operating theatre tearoom and then dinner at the guest house in the compound opposite the hospital, after which we fell into our beds. The patients had no major complications, although a few women had difficulty voiding post-op but that resolved quickly.
Drs Hall and Taylor then went to Fort Portal to train a local gynaecologist for a few days so Gail and I took the opportunity to do some exploring in the Queen Elizabeth National Park, looking at the wildlife and enjoying the views over the Rift Valley.
Fistula camp (14–25 July 2016)
Judith and Hannah arrived from Entebbe for the Fistula Camp and, following arrival, wasted no time in assessing the women who had been arriving for several days beforehand from far and wide. Judith and Hannah are very experienced fistula surgeons with international reputations who have been coming to Kagando for many years.

(left to right): Gail Imm Tan, Barbara Taylor, Judith Goh, John Taylor, Hannah Krause, Jackie Smalldridge, Anuba Rawat
Again, the staff, Harriet and Isaac, had done very well with the screening and logistics of picking up women from various locations so they could be assessed, putting out radio adverts and arranging minivans to pick them up. 96 women were assessed – the potential vesicovaginal fistula (VVF) patients requiring dye tests and careful examination to see where the fistula was. The next day we were back to the operating theatre, where we worked for the next seven days with the two beds in one theatre. Here, 69 operations were done – Judith and Hannah doing most of the VVFs – many of them were repeat surgeries (one patient had had six previous attempted repairs).
Gail and I did mainly the rectoviginal fistulae (RVF) and a few more prolapse repairs. We were able to assist/observe many complicated fistula repairs and were amazed at the complexity of the repairs and Judith and Hannah’s abilities to find tissue planes to close the fistulae when there was so much tissue destruction. Local surgeons, Drs Job and Marvin, also observed and operated on a few cases and hopefully over time will be able to learn the skills to do fistula surgery effectively.

Postoperative patients.
Many of the women had heart-breaking stories, many had no live children, traumatic caesarean sections with ureteric injuries and so on, but the worst was one woman who had a traumatic VVF from the Rawandan Genocide in 1994. One eight-year-old girl fell out of a mango tree and sustained a traumatic RVF. The preoperative patients all had bowel prep, IV antibiotics, as at home, and the RVFs stayed for five days. The VVFs stayed for 14–21 days and had dye tests before discharge to check they were dry after we had departed.
The women were very stoic, managing with paracetamol and diclofenac and the occasional biscodyl for post-op pain and constipation. The postoperative ward rounds look like organised chaos with more than 40 patients to see before the list started in the morning, but we managed not to miss anyone out due to Hannah’s ‘book’, which kept track of everything.
As well as the fistulae and prolapses, we saw a woman with a urethral diverticulum, a woman who needed a fat graft (Martius graft) and two laparotomies were done to re-implant ureters. There were some patients who needed oxybutynin for their detrusor overactivity and many needed bladder retraining and pelvic floor exercises, which was done by the nurses on the ward. We had four patients return to theatre: two RVFs broke down, one VVF leaked post-op and was resutured, and one haematoma was drained from a prolapse repair.
It’s amazing to be part of a team of dedicated and skilful colleagues from whom you can learn so much about what’s possible to do in a resource-poor environment. It certainly puts you to the test professionally and personally.
For more scholarly fistula information, you can download for free in ibooks ‘Practical obstetric fistula surgery’ by Hancock and Browning (Royal Society of Medicine Press 2009).
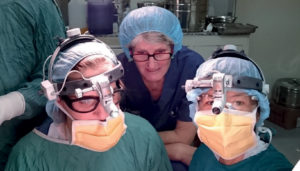
Hannah, Barbara and Judith operating.

Patients with Hannah and Judith






Leave a Reply