‘One of the most pressing challenges facing modern organisations is the need to deliver safe and reliable services under conditions of considerable complexity, change and surprise.’ Carl Macrae 2016 1
Over the past 15 years, PRactical Obstetric Multi-Professional Training (the ‘PROMPT’ course) has become firmly established as a resource for improving organisational safety and resilience in maternity care. In the UK, PROMPT training has been adopted by about 85 per cent of maternity units and, although two very different paths to implementation have been used in Australia and New Zealand (NZ), there is every possibility that with time similar levels of uptake will also occur in Australian and NZ birthing units. This article reviews the development of the PROMPT course in NZ, compares our progress with Australia and considers some of the challenges ahead.
PROMPT began in Bristol, UK, 15 years ago and NZ was an early ‘test-centre’ for the course. The UK faculty visited NZ in 2005 to run a Train The Trainer (T3) Course in Auckland shortly before the publication of the first edition of the UK course manual and the development of a ‘Course in a Box’, containing a trainer’s manual and all course resources. The first Australian T3 course was run in 2010 in Victoria, with an initial pilot program funded by the Victorian Managed Insurance Authority (VMIA). Since 2012, the PROMPT program has been delivered in Australia and NZ by RANZCOG under licence from the PROMPT Maternity Foundation (PMF) UK.
PROMPT has become established in both countries using different models; a ‘mentor model’ is used in NZ, while a series of one-day T3 courses is used in Australia. In 2013, a local Australia and NZ version of the PROMPT course manual and ‘Course in a Box’ was published, based on the second UK edition of the program materials, with the process to be repeated when the third UK edition is released for publication in late 2017.
By the end of 2016, T3 courses had been rolled out to all Australian states and territories. A total of 30 T3 courses have been held and 118 Australian facilities nationwide have undertaken T3 training. At a typical T3 course, a hospital will send a multi-disciplinary team of midwives, obstetricians and anaesthetists (between four and six, depending on the size of a unit). This team will then form the attending unit’s future multi-disciplinary faculty. The RANZCOG T3 faculty have been drawn from a multidisciplinary core of experienced PROMPT teachers and their commitment to the course has been significant, with some facilitating three or four T3 courses across various states annually.
Box 1. Characteristics of a PROMPT course
-
- All staff involved in intrapartum and maternity care within a unit attend; it is not an ‘expert’ course. All courses are multiprofessional, both among the attendees and faculty.
- All staff should attend regularly with the aim of attendance reaching 100 per cent within a unit. PROMPT is not a ‘once a career’ course. Using a real work setting ensures staff know where equipment and medication is kept, and how it
is used. - Simulations are run in-situ on labour ward or a typical place of occurrence for the simulated emergency. A Sim-centre is not used.
- Patient actors are used to ensure interaction between the attendees and sick patient. Expensive whole-body mannequins are not used.
- There is an emphasis on high-fidelity simulation and, wherever possible, real drugs and equipment are used. Simple props are used to simulate blood loss and allow fluid and drug administration.
- There is reflective feedback with one team participating in the simulation and another observing, taking structured notes on clinical and
teamworking issues. Debriefing sessions are used after each drill to explore what went well and why, as well as what could be improved and how. - Running simulations in a real work setting allows staff to test protocols, hospital systems and real-time requests for supplies, such as blood products, medication or operating theatre access. The course can be used to develop standardised processes and tools, such as emergency boxes and protocols for managing particular emergencies.
- There is a strong emphasis on the non-technical skills needed to manage an obstetric emergency, exploring how effective communication, teamworking and situational awareness can increase the effectiveness of multi-disciplinary care in an emergency.
- The course is always locally adapted so that local protocols, equipment and staff are used. The course can be run equally well in a tertiary centre or a midwife-only birthing unit.

Figure 1. Managing a simulated postpartum haemorrhage on labour and birthing suite.
The Australian courses are delivered in local Sim-centres. This has been mainly because of the logistical challenges of running T3 courses within a busy labour and birthing unit. As well as simplifying course organisation for the T3 faculty, it has also had the unintended benefit of convincing most attendees how much easier it is to provide a locally relevant high-fidelity simulation experience in-situ within a birthing unit rather than off site in a Sim-centre. This model does have some significant costs, with each attending unit having to fund attendance at the T3 course (typically about $AU6000 per hospital, plus travel and accommodation for attendees if required). Funding for individual units has come from the Australian Government, state insurers, the State Department of Health or from hospitals themselves. The great majority of those 118 that have attended a T3 course are now running PROMPT training.
In NZ, we have used a mentor model with no T3 courses being run. This has been partly due to an absence of government or insurer funding for units to attend a T3 course and, partly, our much smaller number of birthing facilities making a mentor model more robust and still relatively sustainable. NZ has only six tertiary-level units, 18 secondary-level birthing units and approximately 45 primary midwife-only birthing units (some of these having less than 30 births per year).
Under the mentor model, units send a multi-disciplinary team to attend a PROMPT course in a tertiary centre, thus allowing the potential faculty to both experience a course as attendees and assess how the program might be implemented in their own unit. Faculty from the supporting tertiary unit then travel to help that unit run their first course by supervising them setting up the drills, providing help with adapting slides and lectures for local use and often both delivering some of the introductory lectures and leading some debriefing sessions. Initially, all interested units attended a course in Auckland, but in recent years both Dunedin and Christchurch have provided support to other secondary units and both tertiary and secondary units across the country have helped set up courses in the primary birthing units that they potentially receive referrals from. This more organic approach has presented some challenges, particularly initially with the Auckland faculty visiting almost all of the country’s secondary and tertiary birthing units over a three-year period, but this burden has lessened as ‘local champions’ in tertiary and secondary level units have gained more experience in running the course and have felt comfortable helping other nearby units set up or train new faculty to run PROMPT courses.
Now, in 2017, all NZ tertiary units are running regular PROMPT training, with all except three of our secondary level units running regular PROMPT programs. Many of the secondary level units also support course faculty in local midwife-only units. A total of 380–390 PROMPT courses have now been run in NZ, with nearly 1500 course manuals purchased. Establishing how many individual midwives and medical staff have attended a course is more difficult, but with course sizes ranging from 12 to 30 attendees, it is likely that there have been well over 5000 individual attendances at a PROMPT course in NZ.
It appears that both approaches have been similarly successful in disseminating PROMPT training, but there are some significant challenges for PROMPT ahead. Our three most important challenges are:
-
-
- Maintaining the fidelity of the course, as it is locally adapted by multiple units
- Sustaining the course, both in individual units and nationally
- Funding the course and demonstrating to potential funders that the course is cost-effective
-
Course fidelity
One of the most important aspects of PROMPT training that differentiates it from offsite or expert courses, such as ALSO and MOET, is an emphasis on the course content being adapted to use local protocols, facilities and equipment, with the program also being delivered by a local faculty. There is potential for the quality of a course to deteriorate as local faculty change or lose enthusiasm. Smaller units will continue to need support from time to time from tertiary centres to train new faculty and ensure course fidelity is maintained. Funding to implement the T3 model of course delivery nationally in NZ is likely to be difficult; however, funding for new faculty in smaller centres to visit larger units and mentors to assist those smaller units running their own courses would help maintain course fidelity.
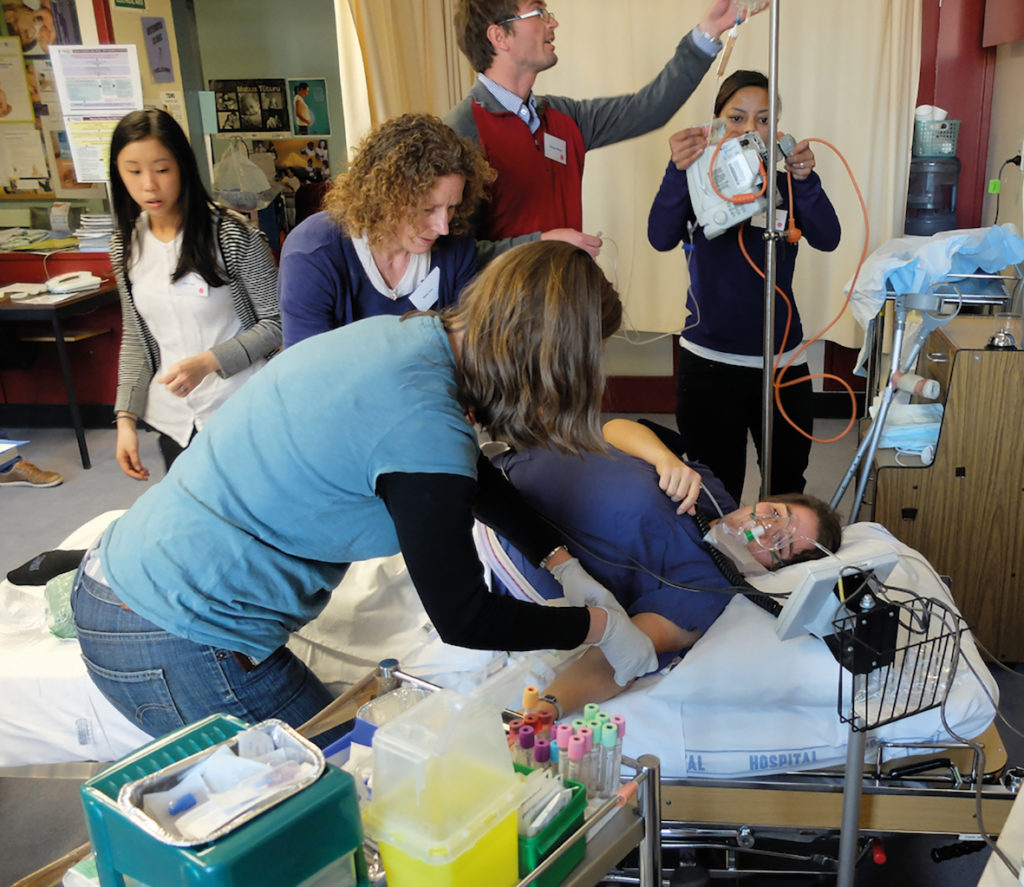
Figure 2. The early stages of a maternal collapse simulation. The team will be moved onto an adjacent mannequin if the actress expires and requires CPR.
Sustaining PROMPT
PROMPT faculty across NZ have reported variable levels of support from maternity management and interest from senior medical staff. The program very much relies on a local clinical champion and committed midwifery educators to maintain enthusiasm and fight for training to be prioritised in times of staff shortage and funding shortfalls. The Perinatal and Maternal Mortality Review Committee (PMMRC) have recommended that all staff providing intrapartum care attend regular multidisciplinary training in the management of obstetric emergencies; however, there is no obligation for any unit to fund or support such training, and as a result, faculty from across the country have at times struggled to continue providing PROMPT training. There is scope for improving local sustainability with more support from a national NZ PROMPT faculty.
Funding and cost effectiveness
One of the biggest challenges PROMPT faces is funding. An expensive offsite or expert-only course attended by two or three staff a year is relatively cheap for a unit to support, but PROMPT – with its underlying philosophy of all staff being trained, being trained together and being trained regularly – is potentially much more costly to implement.
One recent UK study,2 using a micro-costing technique, reported that PROMPT costs €22,000 ($AU 31,000) per 1000 births if 85 per cent or more of all medical and midwifery staff are trained every year. Over 90 per cent of these costs were from back-filling midwifery and medical shifts. A reduced frequency of training or using staff study leave funds would reduce this cost, but could potentially lead to a reduced uptake of training and a reduced effect on improved clinical outcomes. A further challenge for NZ is that a substantial proportion of intrapartum care is delivered by self-employed independent practitioners, leading to debate in many units about whether they should be charged to attend such training or if it should be mandatory and free for all practitioners providing intrapartum care within a birthing facility.
A key question for potential funders is whether or not in-situ simulation training actually ‘works’ and whether there is any evidence that it improves clinical outcomes (Kirkpatrick level 4 evidence), rather than just improving staff knowledge or morale. There is now reasonably robust evidence that PROMPT training can significantly reduce the proportion of cases of shoulder dystocia complicated by a brachial plexus injury,3 reduce the decision to delivery interval for category-one caesarean section,4 reduce the incidence of five-minute Apgar scores of less than five5 and reduce litigation costs for insurers.6 7 There is also increasing evidence that in-situ multi-professional training, incorporating teamwork as in PROMPT, is more effective than offsite training or training in single professional groups.8 9
In NZ, we are in the process of surveying our entire PROMPT faculty nationally, developing a national website and improving communication between local PROMPT educators to support and sustain the course. We also remain hopeful that, with time, PROMPT training will be free to all participants and embedded in all NZ birthing facilities.
References
- Macrae C, Draycott T. Delivering high reliability in maternity care: In situ simulation as a source of organisational resilience. Safety Science. doi: 10.1016/j.ssci.2016.10.019.
- Yau CWH, Pizzo E, Morris S, et al. The cost of local, multi-professional obstetric emergencies training. Acta Obstetrica et Scandinavica. 2016;95(10):1111-9.
- Crofts JF, Lenguerrand E, Bentham GL, et al. Prevention of brachial plexus injury – 12 years of shoulder dystocia training: an interrupted time-series study. BJOG. 2015;123(1):111-18.
- Siassakos D, Hasafa Z, Sibanda T, et al. Retrospective cohort study of diagnosis-delivery interval with umbilical cord prolapse: the effect of team training. BJOG. 2009;116:1089-96.
- Draycott T, Sibanda T, Owen L, et al. Does training in obstetric emergencies improve neonatal outcome? BJOG. 2006;113:
177-82. - Draycott T, Sagar R, Hogg S. The role of insurers in maternity safety. Best Pract Res Clin Obstet Gynaecol. 2015;29:1126-31.
- Weiner CP, Collins L, Bentley S, et al. Multi-professional training for obstetric emergencies in a US hospital over a 7-year interval: an observational study. J Perinatol. 2016;36:19-24.
- Bergh A-M, Baloyi S, Pattinson RC. What is the impact of multi-professional emergency obstetric and neonatal care training? Best Pract Res Clin Obstet Gynaecol. 2015;29:1028-43.
- Cornthwaite K, Alvarez M, Siassakos D. Team training for safer birth. Best Pract Res Clin Obstet Gynaecol. 2015;29:1044-57.






Leave a Reply