My wife, Pam, and I flew into Addis Ababa on 25 May, en route to work for four weeks in the Vision Maternity Clinic at Bahir Dar in the Ethiopian highlands. Addis is a huge bustling shamble of a city of possibly five million people. Dusty smog rises high above the skyline of tower blocks under construction, hiding the mountains that surround the city. Four- and five-star apartments and offices are set incongruously adjacent to shacks of tin and cardboard with woven plant walls and roofs and dirt floors, homes or micro-enterprises; such is any African metropolis.
On this second visit to Ethiopia, we planned a stopover to allow time to visit Catherine and Reg Hamlin’s iconic hospital by the river, the world’s second dedicated fistula hospital (the first in New York in the late 1800s built by Marion Sims). No high-rise steel and glass complex, but mostly single-storey bungalow buildings set among trees and gardens, and pervaded by peace and spirituality. Patients support each other with quiet hope and humour. Catherine, now in her 90s, still walks through the wards each evening.
A one-hour flight onwards brought us to Bahir Dar; 600,000 thousand people living around the southern shore of Lake Tana (80km long and 60km wide), with a year-round pleasant climate. A boulevard centrally planted with tropical trees loops from the airport along the lakeside through the city and onwards towards the castles of Gondar and the Simian mountains (home of the cliff-top-dwelling, grass-eating gelada baboons).
Our new guesthouse was waiting, just 100m from the Vision Maternity clinic, with Meron, the part-time cook and cleaner, preparing a typical Ethiopian lunch with a base of injera, a fermented cooked type of pancake made from tef (the local grain now being recognised in the West as a superfood), and topped with spiced vegetables and lentils. The guesthouse now consists of a kitchen, two bedrooms, and lounge, all opening onto a covered concrete walkway. A real luxury is that bedrooms have ensuite bathrooms, and, to Pam’s delight, a large vegetable garden already growing corn, carrots and tomatoes, for her to get her hands dirty.
I planned a quiet weekend, but somehow the word spread and my first call came on Sunday afternoon for a prolonged second stage requiring assessment and ventouse delivery. The clinic consists of a cluster of buildings connected by rough stone, gravel or concrete open paths, with antenatal, intrapartum and postnatal sections, and adjuvant facilities, such as a pharmacy and HIV clinic nearby. The centre of the complex is a long blue shed, constructed of galvanised corrugated iron walls and roof supported by roughly trimmed stout eucalypt timber. It has a concrete floor covered by well-worn lino. There is a nurses station at one end adjacent to a small room with two beds for high-dependency patients, then 10 ward beds. At the other end is a room with two delivery beds used only for difficult deliveries. There is sterile equipment, and basic resuscitation gear. There is no luxury or modern gadgetry here; the lighting is rather dim and privacy is obtained with threefold screens. Normal deliveries occur in the beds on the ward, adjacent to other patients in labour, breastfeeding mothers or antenatal women with the usual variety of complications. Yet, last year, the clinic was judged the safest place for a woman to give birth in Ethiopia, with no maternal deaths for the last three or four years. The heart of the clinic is the staff, made up of 10 dedicated and incredibly hard-working midwives (12-hour days, six days a week), and a number of associate nurses/cleaners. The midwives are very well trained to WHO-Ethiopian-Andrew Browning standards, commonly attending, at night, ventouse deliveries they judge to be safe, cephalic-presenting twins, and PPHs, without troubling the visiting doctor.

Special delivery suite in the current clinic.
Andrew Browning is an Australian O&G who has taken on the mantle of Reg Hamlin (Catherine’s husband). Now in his mid-40s, he is acclaimed as the world’s finest fistula surgeon. Andrew first visited Ethiopia with his father in 1996 and was invited by Catherine Hamlin to join her, which he did after completing MRCOG training at St George, Kogarah. He remained for four years, operating, researching and teaching. He then moved to Bahir Dar as surgeon in charge of the first regional fistula hospital, while his wife Stephanie started a primary school. He remained six years, operating on patients to whom he administered spinal anaesthetics, eventually doing up to 700 cases a year. He was not blind to the need to improve maternity care to prevent appalling injuries and was rather troubled by practices and outcomes in the large local government hospital. In 2011, he therefore determined to build and attract volunteers to work in a clinic managed by his Australian umbrella foundation – the Barbara May foundation – and this became Vision Maternity. Ructions within management of the Addis Hamlin foundation, and concern for the future education for his two young boys, necessitated a move from Ethiopia. He then found a rather neglected, poorly supervised maternity unit at Selian hospital on the outskirts of Arusha, Tanzania, where his proposal to set up another fistula service was welcomed.
My association with Andrew coincided with his move. With optimistic ignorance of my inexperience in fistula surgery (two or three in my then 30-year career), I had been offering my volunteer time and services to various fistula organisations without success. Andrew answered my ‘cold call’ email with a friendly ‘come over and I’ll find you a job’. I had a very enjoyable four-week visit, handling gynaecological outpatients and surgery, obstetric call when required by a wonderful South African midwife and her staff, and assisting Andrew with fistula work. He kindly assisted me with a small number of fistula cases, but I quickly realised that there is a significant learning curve to obtain best results, that I was working with a genius and could use my general skills to free him to perform miracles.
After two further annual six-week trips, Pam and I were preparing last year for our fourth to Tanzania, when an email from Andrew asked if we would consider instead doing maternity work in Bahir Dar, where a sole visiting obstetrician needed relief. The lifestyle was very different and less Western than Tanzania, but we enjoyed our time greatly and were happy to return this year.
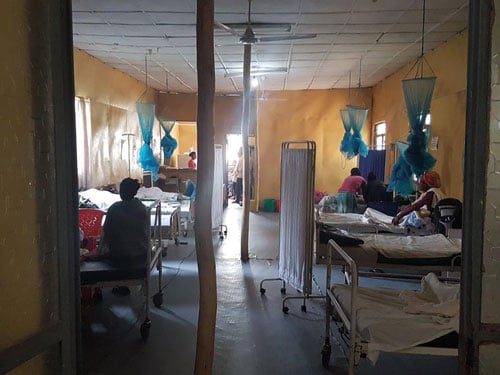
General ward for antenatal, intrapartum and postnatals in the current clinic.
My days began with an 8.30 handover attended by virtually all staff, which was an opportunity to question decisions and teach practical tips, followed by a ward round. A large part of the round is supervising progress of labour (for example, augmentation or rupture of membranes) according to the standard local protocol. I learned to bite my tongue regarding my habit of early rupture of membranes to encourage labour; the protocols are terribly important, contributing a great deal to the excellent outcomes in this clinic, which much of the time is without direct supervision. This means that midwife staff make decisions that in Australia would involve up to senior-registrar-level consultation. When no volunteer is available, staff are required to negotiate decisions and outcomes with doctors at the large government hospital. Patient transfer often involves a three-wheeled covered vehicle known as a bajaj, patient and relatives sitting in the back, certainly not ideal late in an obstructed labour.
I then had time off until patients booked for ultrasound examination, and for consultant clinical decision-making from the antenatal clinic arrived on the ward, usually about 10.30. Two midwives have been well trained to perform dating and fetal growth scans by retired Dutch professor Hans Wolf, a frequent volunteer who can conjure first-world images from an ancient black and white EDAN scanner. As the ‘expert’ (though not having been required to perform complicated obstetric scans in practice in Australia for many years due to the luxury of the availability of expert sonographers) I am asked to corroborate findings, explain reduced fetal movement, check fetal presentation, the quality of the placenta and amniotic fluid, without the benefit of the blood flow methods we have come to rely on in Western obstetrics.
I then relax, apart from booked caesarean sections, until a more clinical flow of patients come for assessment from the afternoon antenatal clinic from about 3–5pm. Most nights require at least one call in and, until I became more ruthless in taking time off, as the only supervising volunteer, I was certainly exceeding ‘safety hours’. Of course, requests to intervene in labour may occur at any time throughout the day.
My tally with a week to go of my four-week visit was 10 ventouse deliveries, nine caesareans and three sets of twins. In the first 10 days, three ‘sphincter tightening’ shoulder dystocias occurred, with one neonatal death. Two intrapartum deaths occurred, one a premature twin with exomphalos. The other occurred to a mother who presented at the clinic and no fetal heartbeat was found. She was fully dilated and I found bradycardic cardiac activity with ultrasound, but had to leave delivery to a midwife as I had a patient anaesthetised for urgent delivery for an abruption. Cord asphyxia due to two knots in two nuchal loops of cord was found. Transfers to the major government hospital included a postnatal thyrotoxic crisis, several women with pneumonia, severe early pregnancy hypertension (the last pregnancy having required termination at 26 weeks). In one 12-hour period, patients included a 31-week placenta praevia patient bleeding, another primip with blood pressure of 240/160, and an unbooked walk-in patient with a fully dilated footling breech.
Simple practical points that have been accepted by staff have included; the ventouse works better when the patient is contracting efficiently, so augment if necessary in the second stage; and documenting the station of the head at abdominal palpation as well as vaginally assists in judging progress. A further manoeuvre I would like to demonstrate is the assisted squatting position for delayed delivery, rather than the upended turtle position, but that will become more practical in the new clinic.
This year, our travels have been curtailed, but Pam and I have enjoyed walks to the Nile Bridge to see hippos, climbed a nearby mountain for views of Bahir Dar and the lake, and walks along the lake shore. Pleasant coffee shops and restaurants are nearby.
We’ve had the privilege of discussions with volunteer ‘Timberologist’, Garry Turland, an eminent builder/developer with a great social conscience, from Bowral/Bondi NSW, who was here for a fortnight to supervise the final fit out of the brand-new maternity clinic, built over the last few years on land behind the blue shed. With at least four times the space of the present building, it is likely to set the standard for Africa and hopefully attract a new generation of volunteers willing to trust their clinical skills to save the lives of mothers and babies.
For more information on volunteering, please visit the Barbara May Foundation website at
www.barbaramayfoundation.com.






Leave a Reply