There is much data, research and evidence on the detrimental effects of violence against women on physical, psychological and emotional health. The impact is significant, not only on patients, but also their families, healthcare workers and the broader community. It is a complex, pervasive issue that affects women across social and cultural divides and, according to research, is increasing in Australia and New Zealand.
The Royal Women’s Hospital (the Women’s), in Melbourne, commonly sees intimate partner violence and its consequences across all its services. The variety of physical health issues that are related to this type of violence can present in a multitude of ways. For example, women may present with higher rates of gynaecological issues, including vaginal and anal bleeding and infections, chronic pelvic disorders, urinary tract infections, fistulas, pain during sexual intercourse and sexual dysfunction. They may also present with reduced reproductive control, increased rates of sexually transmitted infections, pregnancy and complications, and requests for termination of pregnancy.
“The psychological, sexual and controlling behaviours that are associated with intimate partner violence may be less obvious, but are just as significant to the health of women.”
Research shows that hospital and medical professionals are in a unique position to identify and support people at risk of family violence and the Women’s is working to ensure that all medical professionals involved in women’s health understand their role in identifying and supporting women experiencing violence. A toolkit to support healthcare professionals and hospitals effectively deal with this issue has been developed for public use (Figure 1).
The role of the Royal Women’s Hospital
The Women’s is taking a lead in addressing violence against women as a health issue and, as a specialist women’s and maternity hospital, it is uniquely positioned for early intervention to assist women and their children to safety and recovery from violence.
As a state-wide leader in Victoria, the Women’s is collaborating with other health services to build capacity across the whole health system in tackling family violence. It has fostered partnerships with government, academia, the community, other hospitals and the family violence sector. In addition, it is actively participating in, and promoting, research to strengthen the evidence base for clinical care and social support and improve services and programs within the family violence sector.
Tackling the complex and multifactorial challenge of reducing the effect of violence against women has been a priority for the Women’s throughout its history, but never more so than over the past few years, as the focus on addressing violence against women in Victoria has increased following a number of violence-related incidents and deaths.
Since 2015, family violence has been a priority area for the Victorian Government, which has made significant investment in prevention. In February 2015, Victoria was the first state in Australia to hold a Royal Commission into Family Violence, which led to the commitment of $1.91 billion towards addressing family violence in the 2017/18 Victorian budget. In July 2017, it established Victoria’s first-ever agency dedicated solely to family violence reform: Family Safety Victoria.
The Women’s, along with Bendigo Health, was one of the first hospitals in Victoria to develop family violence prevention and response services. The support following the Royal Commission has meant the Women’s role as a leader in this area has now been formalised, enabling it to expand its model to foster greater coordinated activity across Victoria’s public hospitals.
The Strengthening Hospital Responses to Family Violence project
In 2014, the Victorian Government commenced funding the Strengthening Hospital Responses to Family Violence (SHRFV) project, led by the Women’s in conjunction with Bendigo Health. This innovative work aims to develop and implement a framework for embedding within Victorian hospitals the practice of systematically identifying and responding to patients experiencing family violence.
The SHRFV project covers all elements of developing and supporting a whole-of-hospital approach to implementing a family violence program in any hospital setting in Victoria. Based on international best practice, the SHRFV model (Figure 2) has two overarching principles and five key implementation elements. It aims to deliver a whole-of-hospital response to violence and achieve better outcomes for women, children and families in Victoria.
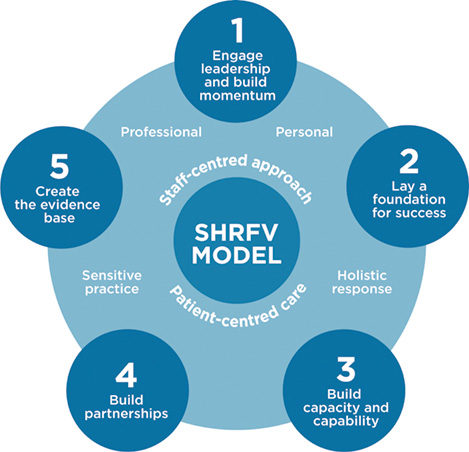
Figure 2. SHRFV Model Diagram
Core to SHRFV is creating a safe and welcoming physical space for women and staff who might be experiencing violence, and providing the right training, tools, support and structures to enable hospital staff to identify and sensitively enquire about family violence.
Some of the practical aspects of the SHRFV program include the following:
- Training staff on how to have the confidence and skills to identify, respond to and refer on women experiencing or at risk of violence.
- Ensuring physical sites are safe and welcoming environments.
- Supporting and mentoring other hospitals to be able to identify and respond to family violence, particularly through the creation of a toolkit that contains a host of information, training programs, adaptable marketing material, and policy and procedures concerning the prevention of violence against women and the role of hospitals. This toolkit has been specifically developed to be adaptable to any hospital and applicable in any healthcare setting.
One of the key tenets of the SHRFV project is that healthcare professionals are not expected to become ‘experts’ in family violence prevention. Rather, it aims to encourage and give confidence to health workers so they feel able to sensitively enquire and support women experiencing, or at risk of, violence, and know where to refer them for further support.
Beyond the SHRFV project
The Women’s continues to contribute to the prevention of violence against women in other ways, such as by supporting staff who may be at risk of, or experiencing, violence; supporting managers; and undertaking research into family violence.
In 2016, it implemented a workplace support program for employees affected by family violence. The program includes training for colleagues and managers, human resources policies and procedures to better support staff experiencing violence, and the introduction of family violence leave to help individuals to manage issues and appointments associated with family violence.
The hospital also established a Centre for Family Violence Prevention, a hub for researching interventions, including identification tools, early intervention and therapeutic responses, to assist women experiencing family violence. In 2016, Prof Kelsey Hegarty was appointed Australia’s first chair of Family Violence Prevention, a joint appointment by the Women’s and the University
of Melbourne.
Early in 2017, the Women’s CEO, Dr Sue Matthews, was appointed the hospital representative to Victoria’s Family Violence Steering Committee, which provides specialist advice on the development and implementation of policies, strategies and programs that seek to address family violence in Victoria. The Women’s has also recently been appointed as one of four Victorian hospitals to trial routine screening for family violence in an antenatal setting.
“The Women’s believes that prevention and intervention of violence against women should be core business to all health professionals.”
The goal for the next four years is to continue to develop and implement a sustainable, whole-of-hospital response to violence against women right across Victoria. This will be achieved by aligning and prioritising the safety and wellbeing of women exposed to violence professionally or personally and educating and supporting health professionals to enhance their capacity, capability and confidence to practice sensitive inquiry into violence and appropriately refer.
Family violence is a complex issue, but we encourage all healthcare professionals to take a look at the toolkit that has been developed by the Women’s, Bendigo Health and other respected hospitals to provide practical support and tools.







Leave a Reply