An acute abdomen in pregnancy is rare, but a ruptured tubo-ovarian abscess should be considered despite being a rare occurrence in pregnancy.1 Rupture can occur in approximately 15 per cent of cases of tubo-ovarian abscess.1 There are a few case reports of ruptured tubo-ovarian abscess in pregnancy.2 3 4 5
Case report
A 24-year-old woman (G3P2) had a history of two normal vaginal births. Her previous pregnancies were uncomplicated and she had no significant medical history. During her current pregnancy, she had attended two antenatal visits where her fundal height was consistent with her dates. A venereal disease research laboratory (VDRL) test had been collected at the first visit and shown to be positive with a titre of 1:4. The first dose of benzathine penicillin had already been given.
She presented to the emergency department in the National Referral Hospital, Solomon Islands, at approximately 32 weeks (based on her last menstrual period) at 6pm with severe abdominal pain. The pain was worse in the right upper quadrant and right iliac fossa. She also complained of fever. There was no dysuria or bowel symptoms and no nausea or vomiting. She denied any trauma or falls. There was no history of ruptured membranes or per vaginal (PV) bleeding.
On examination, her blood pressure was 90/59, pulse 98 and temperature 38 degrees. Her abdomen was markedly tender on the right side with bilateral renal angle tenderness. Fundal height was 32cm with the fetus in cephalic presentation, not engaged. No contractions were palpated. On vaginal examination the cervix was closed, with some tenderness noted in the right fornix. The fetal heart rate was normal.
At this stage, the differential diagnosis was appendicitis, placental abruption, urinary tract infection/pyelonephritis and torted ovarian cyst. A surgical consult was requested and dexamethasone was administered for fetal lung immaturity. The surgeons requested FBC, UEC, LFT, MPS (malaria parasite screen) and renal/obstetric ultrasound.
Further review at 1:30am by surgeons was that the woman had likely pyelonephritis and IV antibiotics were commenced.
The following morning, she had generalised abdominal tenderness and a tense uterus. She was diagnosed as having an acute abdomen in pregnancy. The CTG showed a baseline of 155, variability 5–7, no accelerations and complicated variable decelerations down to 50bpm (unprovoked).
An urgent abdominal ultrasound confirmed a large placental abruption with a live fetus (measurements not done). She was taken to theatre at approximately 12pm for urgent caesarean section. A general anaesthetic was performed using suxamethonium, thiopentone and vecuronium.
Upon entry into the peritoneum, there was a large amount of pus oozing through the incision site, thought to be from a ruptured appendix. Triple IV antibiotics were commenced (metronidazole, cephazolin and gentamicin). The surgeons were called to remove the appendix which, interestingly, appeared normal. The abdomen was irrigated with saline. A lower segment caesarean section was then performed. The liquor appeared clear and the baby was born in fair condition. The uterus was closed and exteriorised to examine the tubes and ovaries. A large mass was seen on the right ovary/tube, measuring at least 10cmx6cm. The pfannenstiel incision was converted into a midline laparotomy incision. The remainder of the bowel was examined by the surgeons.
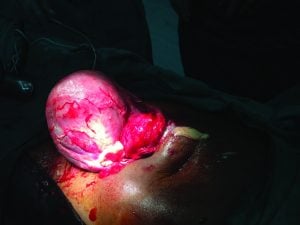
Figure 1. Right tubo-ovarian abscess.
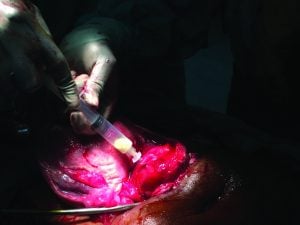
Figure 2. Drainage of ovarian abscess.
The tubo-ovarian mass was aspirated and shown to contain thick purulent discharge. The mass was incised and the loculations broken up. It was marsupialised, washed out and a drain inserted upon closing the abdomen.
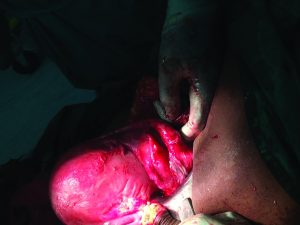
Figure 3. Post-incision and drainage.
Post-operation, mother and baby recovered well. The intra-operative wound swab subsequently grew coagulase-negative staphylococci. Mother and baby were discharged one week later.
References
- Beigi R. Management and complications of tubo-ovarian abscess. Up to date. July 2016.
- Piegzová A, Unzeitig V, Ceska Gynekol. Tubo-ovarian abscess in the 39th week of pregnancy (case report). Ceska Gynekol 2017 Fall;82(4):322-326.
- Han C, et al. In vitro fertilization complicated by rupture of tubo-ovarian abscess during pregnancy. Taiwan J Obstet Gynecol. 2015 Oct;54(5):612-6. doi:10.1016/j.tjog.2015.08.017.
- Davey M, et al. Ruptured tubo-ovarian abscess late in pregnancy. A case report. S Afr Med J. 1987 Jan 24;71(2):120-1.
- Derby B. Ruptured tubo-ovarian abscess in pregnancy. Sex Transm Dis. 1986 Jul-Sep;13(3):177.







Leave a Reply