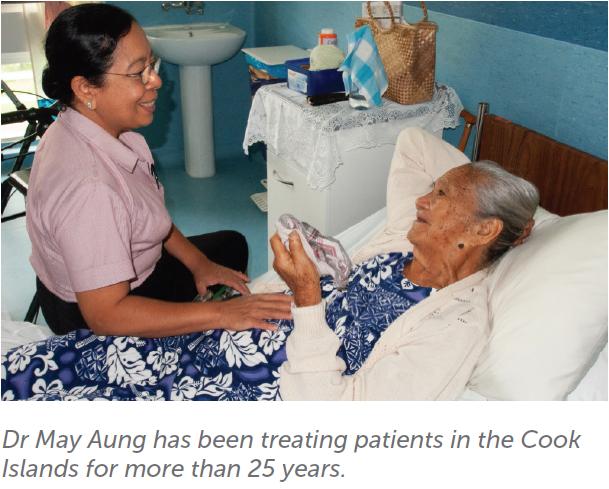
After more than 25 years of outstanding practice in the Cook Islands, Dr May Aung will retire in June. We spoke to Dr Aung about her career in healthcare and about practicing O&G in a remote and challenging Pacific location.
Dr May Aung moved to the Cook Islands in 1989, joining her husband Zaw Aung, who had been working there as a United Nations volunteer. They were initially based in Mangaia, the southern-most island. A general practitioner in Myanmar since 1975, May soon found herself working with patients there, despite not holding any official appointment.
In 1993 she took a position on Aitutaki, the secondlargest island, working there until 2001, when she was asked to move to the largest island Rarotonga, to work more closely with the Ministry of Health. May has been in Rarotonga since then, serving as head of her department from 2005, and eventually becoming Director of Hospital Health Services in 2017.
Obstetrics and gynaecology had always been an area of interest for May, ever since she was attached to an O&G department after completing her internship. However, in the Cook Islands it became increasingly central to her work, particularly given that she was the only female doctor in the country for much ofher time there.
“I wanted to do O&G all the time,” May recalls. “But when I got to the Cook Islands, it pushed me more because I felt responsible as the only woman doctor in the country. And the women felt very comfortable with me looking after them.”
In 2004, May became the first non-Cook Islander to be awarded a scholarship through the New Zealand Scholarship Scheme, completing a Diploma in Gynaecology and Obstetrics at Fiji National University (FNU). There was the option for further study, but May was facing too many demands back in the Cook Islands.
“I was qualified to continue my Masters, and FNU waited for me for five years,” says May. “But sadly, the Cook Islands wouldn’t let me go back because there was no-one to carry on the services in the country. They wouldn’t let me leave to continue my studies because there was no-one to work.”
And there has indeed been a lot of work. In Aitutaki, May oversaw around 50 deliveries each year; after moving to Rarotonga, her team was dealing with 250 to 300 births annually. May has been on call 24/7, attending every delivery, and she speaks with pride about the fact the Cook Islands has maintained a zero maternal mortality rate since 1995.
Alongside countless successful births, there have been other achievements along the way. May cites a mammogram screening program that she is currently overseeing, which follows on from a highly successful overhaul of the Islands’ cervical screening set-up.
“When I started, we were using conventional smears on glass slides,” she explains. “But now we’re doing HPV screening, which one only has to do every five years, and this improves our screening uptake. How did I get to that? I went to do a presentation in March 2019 in Auckland, and I met the New South Wales Australian team, and they supported me to progress to cervical cancer screening by HPV.”
These achievements have taken place amid the considerable challenges of operating in the Cook Islands. The country consists of 15 islands spread across 2.2 million square kilometres of ocean, with transport links extremely limited, especially among the more remote northern islands. Staffing is another issue, with a shortage of midwives on many of the islands.
May describes one case of a woman with a ruptured ectopic pregnancy in Rakahanga, an island with no airstrip, necessitating a three-hour boat trip to receive treatment. In another case, May had to fly to Pukapuka to perform an emergency Caesarean. She took a limited team, as well as two drums of aviation fuel because there was none on the island for the return flight.
Challenges such as these are a constant for May:
“Currently I have four pregnant mothers who are due this week. I’ve been trying to transfer them, but there is no fuel for the flight to go up, and one flight is down because of a brake problem. And my heart is very heavy because one is a gravida nine mother in Pukapuka.”
These challenges inevitably place an intense emotional burden on May: “It is very lonely because you are the only person practicing O&G in the country. You are 24/7 on call, and I never failed to attend one delivery in my career. And sometimes, you are so tired, but you still have to continue your clinics.”
Nonetheless, May draws great satisfaction from her work: “Because you have saved many lives, and the appreciation and gratitude from the families, I think it’s worth all the stress and the hard work. The children I delivered in Aitutaki and in Rarotonga, they’re now having babies, and I have delivered them. And when I go on the road, they are calling me ‘Dr May, Dr May’, and they say ‘Oh, my mother told us you delivered me.’ It really makes me happy.”
For women O&G specialists considering working in the Pacific region, May advises: “It is a very hard and challenging career, but it is worth it because you are saving lives and looking after not only one patient, but the whole family. I’ve made lots of friends and I was able to help people to improve their health and change their family status through doing O&G.”
Recently, May has been heavily involved in a project quite removed from her usual O&G practice. Since late 2020, she has been instrumental in the rollout of the COVID-19 vaccine in the Cook Islands, and as she recounts it, her participation was unexpected.
“I just got pulled into this thing,” she explains. “Over Christmas 2020, the then-Secretary of Health decided to leave suddenly. I was told on the 24th, and the new secretary was a non-medical person. So, I was dragged along to Cabinet meetings with this new secretary, and the Prime Minister asked us, ‘Have you finished your deployment and COVID vaccination plan?’ And I had no knowledge. This is not my area; this is a public health area.”
Despite this, May agreed to help. She started to ask questions and gather information, reaching out to bodies such as UNICEF, the World Health Organization (WHO) and the New Zealand Ministry of Health for support. By Easter 2021, May and her team had put together a plan.
“We started vaccinations on 17 May on Rarotonga,” she continues. “And we’ve been going to the outer islands to give the first dose, second dose and the booster. We went around each village talking to the people before we gave the immunisation. So, the uptake was very good. We’ve covered 98% of the 12- plus population in Cook Islands. With the five to 11 age group, we are around about 82%.”
It’s an astonishing success that comfortably surpasses the efforts of many far wealthier nations – Australia and New Zealand included. But May is characteristically humble.
“This was not only the Ministry of Health effort – it was a community effort,” she says. “We were supported by all other agencies and ministries, and the traditional leaders, the church leaders, the youth, the NGOs like the Red Cross. So, I think it is a united achievement by all the people of the Cook Islands.”
May’s remarkable work in the vaccine rollout serves to enhance an already extraordinary legacy during her time in the Cook Islands – one that her colleagues keenly endorse. Dr Martin Sowter is one such colleague who has worked closely with May, regularly visiting the Cook Islands for nearly 20 years to mentor colleagues and build O&G capacity there.
He is also an obstetrician and gynaecologist based in Auckland, and a member of RANZCOG’s Global Health Committee.
“Every doctor encounters a couple of colleagues over the course of a career that they regard as personal ‘superheroes’ – an embodiment of everything that makes a great doctor,” says Martin. “For me, May has been one of those people. Her quiet, determined, meticulous and completely caring approach to her work and her patients has kept the women of the Cook Islands safe from the start of their pregnancies through to old age. In her role as the nation’s only

O&G specialist, she’s had a workload and range of responsibilities that most Australian and New Zealand colleagues would find crushing.
“More recently as the director of hospital services, she has been a master at making politicians believe that a good idea was their idea and then ‘getting stuff done’. I still fondly remember meeting her in Auckland a few weeks before their COVID-19 vaccine rollout, when the New Zealand program was still bogged down by committees and dithering. New Zealand experts were worried about cold chains, vaccine supplies, and wondering if the Cook Islands could really run the vaccination program.
“May and her team just threw everything at the project and rolled the program out across the nation’s 13 inhabited islands in weeks, with possibly the highest and fastest vaccine uptake in the world. May is far too modest to take any credit for this but she was absolutely crucial to the success of their COVID vaccination campaign.”
Dr Amanda Noovao-Hill grew up in the Cook Islands. Now based in Queensland, she is currently Head of Secretariat for the Pacific Society for Reproductive Health (PSRH), of which May is a member. Last year May and Amanda secured funding for two midwifery leaders and a medical officer to represent the Cook Islands at last year’s PSRH conference in Samoa – though unfortunately, due to travel logistics and COVID, the three clinicians were unable to attend.
In her capacity as Clinical Associate Professor in O&G at the FNU’s College of Medicine, Nursing and Health Sciences, and as a former RANZCOG Global Health Committee member, Amanda often provided support for May in efforts to strengthen O&G service and training in the Cook Islands.
Strategies implemented by May and Amanda included: audio and video conferencing with the Rarotonga O&G Unit and the outer islands clinical teams providing advice and support; enabling onsite training of a local junior doctor and a postgraduate trainee; assisting with recruitment of regional O&G support; and facilitating training opportunities for other health-related specialties.
“Thank you May for your love, sacrifice and service to the Cook Islands, and your professional collegiality to the regional academic institutions and our professional societies,” says Amanda. “Kia manuia I toou akangaroianga. Te Atua te aroa.”
Finally, May is on the verge of stepping away from O&G. She first broached the idea of retirement three years ago, but the Ministry kept persuading her to stay on. However, May is now adamant she will not extend any further. It’s time for a well-earned rest.
“I don’t think I will do anything,” she laughs. “I will not be doing anything in regard to medicine. I will just enjoy life. I really don’t know what to do yet – maybe some planting flowers, or fabric painting, which I enjoy very much.”
And as for the Cook Islands?
“I will stay for a while, but we will definitely have to go back to Myanmar at some stage. I have family there. I have my house. So, I will have to leave the Cook Islands, which will be sad. But I have been trying to prepare myself.”







Leave a Reply