
The death of a baby before, or shortly after, birth is one of the most devastating outcomes of pregnancy. The past two decades have seen a spotlight clearly shone on stillbirth, both globally and nationally. In 2016, the National Health and Medical Research Council funded the Centre of Research Excellence at the Mater Research Institute in Brisbane (the ‘Stillbirth CRE’), and in 2017 a Senate Inquiry was held into Stillbirth Research and Education that led to two round-table meetings at Parliament House. This Federal government-led activity ultimately led to the release of a Stillbirth National Action and Implementation Plan in December 2020. Although much has been achieved already, the important work of the Stillbirth CRE is ongoing, and we were rewarded in 2021 by being refunded for another 5 years. Two major components of our work are developing and helping to implement strategies for stillbirth prevention and promoting best practice care after stillbirth and neonatal death, which includes respectful and supportive bereavement care.
In 2018, the Stillbirth CRE was awarded an NHMRC partnership grant, working with the three largest health jurisdictions (Queensland, New South Wales, and Victoria), to introduce the ‘Safer Baby Bundle’, a bundle-of-care package designed to improve practice in maternity care, and aimed at reducing late gestation (>28 weeks) stillbirth by at least 20% by 2025. The five elements of the strategy are shown in Figure 1, and this program has been delivered to maternity services and health professionals through the development of position statements based on the best evidence, a range of resources for clinicians and women, and an e-learning program (which has now been completed by over 10,000 clinicians).
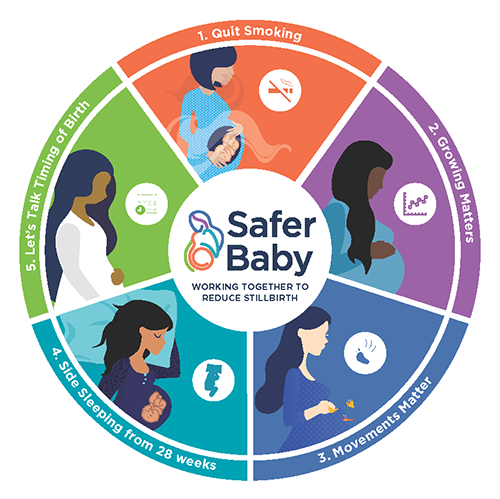
Figure 1: The five elements of the Safer Baby Bundle.
These five elements were chosen specifically based on evidence-practice gaps across Australia and have the potential with improved care to not only reduce stillbirth but reduce neonatal morbidity and mortality plus improve maternal health outcomes. In partnership with the Australian Preterm Birth Prevention Alliance, the timing of birth element of the Safer Baby Bundle is linked to the safe prevention of preterm and early term birth in Australia. Shared decision-making and improved surveillance for women with risk factors aims to ensure that pregnancies continue where it is ‘safe to stay’ and that planned births are limited to situations where earlier timing may prevent stillbirth. In working together, these two National Quality Improvement Initiatives cover the two most important outcomes of pregnancy. Over the past 2 years government funding has supported the co-design of a set of new resources to support timing of birth and stillbirth prevention discussions with our first nations and migrant and refugee families.
The SBB was rolled out in the three initial states in very different ways. Victoria began in 2019 using a collaborative model in partnership with the Institute for Health Improvement. Queensland launched the program in 2020 with all maternity services signing up to the program, and statewide meetings were held to share ideas about implementation. NSW chose a small number of Local Health Districts (LHDs), based on their stillbirth risk profiles. In 2021, the CRE received additional MRFF funding to roll-out the program nationally and all states and territories have now become involved to different degrees in the implementation of the SBB. Clearly, in the 4 years since we started program, the COVID-19 pandemic has been a major distraction for maternity services, as well as having both direct and indirect impacts on stillbirth rates. Regardless, early data from Victoria, NSW and Queensland are showing positive signs in terms of some of the process and balance measures, including improved detection of FGR and reductions in early term planned birth, as well as slowing of late stillbirth rates, despite COVID-19. Nationally, the stillbirth rate >28 weeks of pregnancy is decreasing and has fallen from 2.9 to 2.4 per 1000 births between 2012 and 2020. A full evaluation of the impact of the SBB both locally and nationally is currently underway, and the development work towards the next iteration of the SBB has already begun. Qualitative work with both healthcare professionals and pregnant women indicates that the program is already improving conversations around stillbirth, reducing stigma and improving women’s experience of care.
In an ideal world, all perinatal deaths would be prevented, but this is an unrealistic goal and the best we can achieve is to minimise the number of preventable stillbirths and neonatal deaths. Reducing the overall impact of perinatal loss on families, and the wider community, is one of the goals of respectful and supportive perinatal bereavement care. The Perinatal Society of Australia and New Zealand (PSANZ) has developed a classification system for both perinatal and neonatal deaths, which has been published as part of a clinical practice guideline for care around stillbirth and neonatal death, and this has been available since 2005 with regular updates. Recently, a multidisciplinary team of researchers, clinicians and parents have worked together to produce an updated, comprehensive, evidence-based guideline, which is currently awaiting NHMRC endorsement. This new guideline (the fourth update) will include new chapters on Perinatal Palliative Care and Care in Subsequent Pregnancy, as well as new advice on investigations after stillbirth and neonatal death. The diagram in Figure 2 illustrates the proposed framework for providing best practice perinatal bereavement care in the guideline plus accompanying resources for parents.
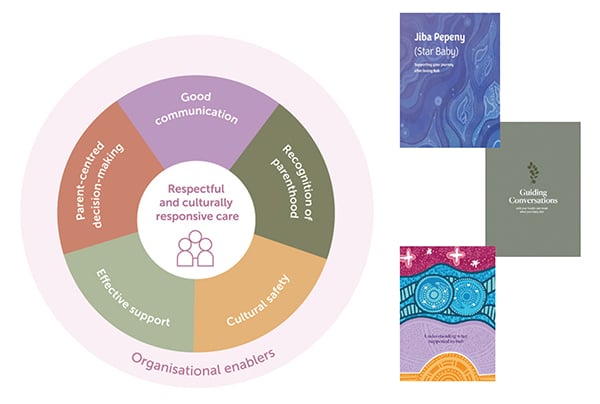
Figure 2: Proposed framework for providing best practice perinatal bereavement care (left) accompanying resources for parents.
Complementary to the Care after Stillbirth and Neonatal Death Guidelines, The Australian Commission on Safety and Quality in Health Care published The Stillbirth Clinical Care Standard in November 2022. This clinical care standard describes clinical care to support the prevention and investigation of stillbirth, and bereavement care for all forms of perinatal loss, including stillbirth, miscarriage, termination of pregnancy and neonatal death. It contains 10 quality statements and seven indicators to reduce unwarranted variation and improve the appropriateness of care for stillbirth prevention, and the quality of bereavement care following perinatal loss. Clinical care standards help support the delivery of evidence-based clinical care and promote shared decision-making between patients, carers and clinicians. They aim to ensure that people receive best-practice care for a specific clinical condition or procedure, regardless of where they are treated in Australia.
Once endorsed, the Stillbirth CRE, working in conjunction with PSANZ, will be developing an implementation plan for the new guidelines, which will include a perinatal bereavement pathway toolkit for clinicians. If we can’t prevent all stillbirths and neonatal deaths, we can try to reduce the impact on families by providing respectful and supportive bereavement care, which begins at the time of diagnosis of fetal or neonatal (or when it is realised that death of a baby is inevitable) and continues on to care in the next and sometimes subsequent pregnancies. An educational program, which is available both as a face-to-face workshop or online, has been developed and is named Improving Perinatal Mortality Review and Outcomes via Education (IMPROVE); it is primarily designed to inform clinicians about the PSANZ guidelines. The CRE has recently received additional Federal government funding to update this popular educational package and include information on cultural safety and inclusiveness for Aboriginal and/or Torres Strait Islander families and South Asian or African-born families, miscarriage, care in subsequent pregnancies and the wellbeing of care providers. The last point is in recognition of the fact that those of us who deal with perinatal death on a regular basis, and who are frequently caregivers to those families who have experienced the loss, can be impacted significantly themselves and might also need support.
As a community, and as a caring group of health professionals, we have come a long way since the days when stillbirths were not discussed or even acknowledged, the identity of the baby not recognised (which denies parenthood), and little attempt made to investigate and try to find out the reason why it happened. It is not long ago that there was stigma attached to the death of a baby, and women were often blamed for this adverse outcome of pregnancy. Indeed, this is still the case in many countries around the world where a common response to stillbirth will be to find someone or something to blame, and it is often the mother herself. Working together with bereaved parents, the Stillbirth CRE and our many partners have made a significant difference, but as always there is so much more to do!








Leave a Reply